Document Type : Original Article
Authors
1 Master of Pharmacy Study Program, University of Indonesia, Depok, Indonesia
2 Laboratory of Microbiology, Department of Pharmacy, University of Esa Unggul, Jakarta
3 Pharmacy Installation, Fatmawati General Hospital, Jakarta, Indonesia
4 Department of Cell Biology and Biomolecular, Faculty of Medicine, Indonesian Defense University, Bogor, Indonesia
Abstract
Background: High use of antibiotics in sepsis patients can lead to irrational use of antibiotics. Irrational antibiotic therapy in septic patients in the ICU increases the mortality rate in the hospital. Efforts to maximize the rational use of antibiotics are one of the pharmacist's responsibilities.
Aim: This study aims to evaluate the quality and quantity of antibiotic use in sepsis patients in the Intensive Care Unit (ICU) ward using the Gyssens and ATC/DDD methods and to evaluate the effect of pharmacist intervention in improving the quality of antibiotic use and therapeutic outcomes.
Materials and methods: The research was carried out prospectively during the period of August-November 2018 using a one-group pretest-posttest pre-experimental study design. Recommendations are given to prescribers regarding the problem of inappropriate use of antibiotics.
Result: Qualitative evaluation using the Gyssens method found that rational use of antibiotics in sepsis patients was 85.1% and 14.9% were irrational. The interventions increased the accuracy of the use of antibiotics (0% to 64.7%), reduced the problem of choosing antibiotics (88.2% to 32.4%), the problem of the duration of antibiotic administration (5.9% to 0%) and the problem of the route of administration of antibiotics (5.9% to 0%). The results of the quantitative evaluation obtained the value of the use of antibiotics, namely 63.8 DDD/100 days of treatment, with the greatest value for meropenem antibiotics, namely 32.9 DDD/100 days of treatment.
Conclusion: There are differences in the therapeutic results between the quality of rational use of antibiotics and the quality of irrational use of antibiotics in the ICU ward of Fatmawati Hospital.
Graphical Abstract
Keywords
Introduction
Sepsis is defined as life-threatening organ dysfunction caused by the body's irregular response to infection. Septic shock is considered as a subset of sepsis in which underlying circulatory, cellular, and metabolic abnormalities contribute to a greater risk of death than sepsis alone [1]. Sepsis was identified as the most expensive condition in hospitals in the United States in 2011, accounting for 6.2% of the total cost for all hospitalizations, or USD 23.7 billion annually. Sepsis is a time-dependent condition where an hourly delay in diagnosis or in starting an effective treatment is associated with an adverse outcome and higher costs [2]. Member countries of the World Health Organization (WHO) state that improving the prevention, recognition, and treatment of sepsis is a global health priority [3]. Sepsis is one of the most common causes of death in the ICU, and its incidence has more than doubled over the last 10 years. According to data from the Surviving Sepsis Campaign (SSC), the death rate from sepsis is 41% in Europe, 28.3% in the United States, and 18-20% in Australia and New Zealand [4]. Delay in the appropriate administration of antibiotics is associated with a significant increase in mortality, and antibiotics should be started within the first hour after the diagnosis of sepsis is known. Empiric antibiotics should be broad-spectrum covering all possible pathogens. Selection of empiric antibiotics should consider the site of infection, previous use of antibiotics, local pathogen susceptibility patterns, immunosuppression, and risk factors for resistant organisms [5]. Empirical antimicrobial therapy should be tapered after identification of the pathogen and susceptibility is obtained, or discontinued if the decision is made that the patient does not have infection. The relationship between empiric antibiotic administration for suspected infection and definitive antibiotic management is an important aspect of quality sepsis management. If the infection is later proven not to be present, the antimicrobial should be discontinued [6].
Inappropriate antibiotic therapy in sepsis has been reported, which has an incidence rate of 15% to 30% in patients admitted to the ICU and is associated with increased in-hospital mortality. In a retrospective study of 5,715 patients with septic shock spanning 22 medical institutions in 3 countries, initial inappropriate antimicrobial therapy occurred in nearly 20% of all patients, with 18.8% occurring in those with community-acquired infections and 28.4% in those with nosocomial infections. These data indicate that the use of antibiotics must be monitored and used wisely to obtain rational quality and quantity of use. To increase the rational use of antibiotics, it is necessary to evaluate the use of antibiotics in various healthcare facilities, especially in hospitals. This study aims to evaluate the quality of antibiotic use qualitatively using the Gyssens method and quantitatively using the ATC/DDD method in the intensive care unit (ICU) of Fatmawati Hospital. Multidisciplinary teams involving pharmacists in the ICU have been proven to reduce mortality in sepsis patients. Pharmacists can act as a source of drug information, speeding up verification and procurement processes and offering advice on how to better manage patients. Pharmacists can provide recommendations regarding dosage and appropriateness of antibiotic selection in sepsis patients. A sepsis management team involving a pharmacist can improve the antibiotics appropriateness used by patients. Several studies show that intensive care units with pharmacists are associated with a 4% reduction in mortality in sepsis patients compared with those without pharmacists [7].
Materials and Methods
The research design used a one-group pretest-posttest pre-experimental study design with a prospective approach, namely research conducted with one group that was given an intervention, and then observations were made before and after the intervention. The intervention was carried out in the form of recommendations on the irrational evaluation results of antibiotics using the Gyssens method by researchers through the intensive care pharmacist to the doctor in charge of services in the ICU room in writing on the integrated patient development record sheet and orally. The data was taken from the medical records of patients who were undergoing treatment in the intensive care unit (ICU) of Fatmawati Hospital. Sampling was carried out in total for all sepsis patients treated in the ICU in the period from August until November 2018. The inclusion criteria were sepsis patients treated in the ICU who received antibiotic therapy and adults over 18. Exclusion criteria were therapy was stopped because the patient was forced to go home, and patient data was incomplete. The minimum sample size was calculated using the World Health Organization (WHO) minimum size table with a test power of 80%, a degree of confidence of 95% and the proportion of septic patients using antibiotics in the ICU was 85%-95% [6]. In this study, a minimum sample size of 62 was required. Criteria used to classify rational or irrational use of antibiotics using the Gyssens flow diagram which is divided into categories 0 to category VI. The quality of antibiotic use was evaluated to see the accuracy of the use of antibiotics with the Gyssens method with category 0 (appropriate and rational use of antibiotics), category I (incorrect timing of antibiotic administration), category II (inappropriate dose, route and interval of antibiotic administration), category III (inappropriate duration of antibiotic administration), category IV (inappropriate choice of antibiotics), category V (no indication of antibiotic administration), and category VI (incomplete data so antibiotic use cannot be assessed) [8]. The quantity of antibiotic use was calculated based on the DDD method/100 patient-days of hospitalization [9]. In evaluating the use of antibiotics quantitatively, the WHO has established the ATC/DDD system as an international measurement standard. The aim of ATC/DDD is as a tool to monitor and research drug utilization in order to improve the quality of drug use. The ATC/DDD method is one of the recommended methods for quantitatively evaluating the use of antibiotics in hospitals. DDD is defined by the WHO as the assumed average maintenance dose per day for a drug used for its primary indication in adults. The research was conducted after obtaining approval from the relevant agencies. Data analysis was performed using the SPSS program with the Chi-square test to test whether there was a relationship between the type of antibiotic, the type of antibiotic therapy, the number of antibiotics used by patients, the number of drugs used by patients, doctors, and length of stay on the quality of antibiotic use. The Wilcoxon test was used to test changes in the results of the Gyssens category before and after the intervention. The Mann-Whitney test was used to test whether there is an influence between the quality of rational use of antibiotics and the quality of irrational use of antibiotics on the therapeutic outcome.
Results and Discussion
The study was conducted on antibiotic regimens prescribed by doctors in the Intensive Care Unit (ICU) room of Fatmawati General Hospital during the period August-November 2018. During the study period, 239 antibiotic regimens were obtained from 73 patients. A total of 11 antibiotic regimens from 4 patients were excluded because the patient moved to the VIP room (orchid) where there were limitations in following developments and the use of antibiotics by patients. The results of evaluation using the Gyssens method of 228 antibiotic regimens were 194 (85.1%) 0 (rational) antibiotic regimens and 34 (14.9%) antibiotic regimens in categories I-V (irrational) with 22 recommendations received by doctors and 12 rejected recommendations. These results are not much different from the research conducted by Rachmawati where the evaluation of rational antibiotics was 89% and 11% irrational [10]. Characteristics of septic patients who received antibiotics can be seen in Figure 1. This study showed that out of a total of 69 patients with a diagnosis of sepsis who were treated during the study period, all received antibiotic therapy. This is not much different from the results of a study conducted by Kayambankadzanja which stated that the majority of ICU patients received antibiotic prescriptions (81.6%), and almost all treatment was started empirically, with broad-spectrum antibiotics [11].
The age group that most suffer from sepsis in the ICU is the age group of 18-64 years, which is 65.2%, followed by the age group ≥ 65 years, which is 37.8%. These results are not much different from the research conducted by Kamal where the largest age group was 18-30 as 38%, 41-65 as 42%, and over 65 as 20%. Sepsis is more common in younger individuals in developing countries and the pathogenic organisms that tend to be responsible are gram-negative pathogens 58%, gram-positive 38%, and fungi 4% [12].

Figure 1: Characteristic of patients receiving antibiotics (n = 69)
The incidence of sepsis by sex found that the prevalence of sepsis in women is lower (43.6%) than in men (56.4%) [13, 14]. The length of patient stay in the category of more than 11 days, is not much different from a cohort study conducted in France where the average length of stay in hospital for sepsis patients was around 17 days. Prolonged hospital stays, especially in intensive care units, can lead to increased mortality and patient care costs [15]. The sources of infection causing sepsis acquired in this study were abdominal infections at 44.9%, lung infections at 40.6%, urinary tract infections at 4.3%, gangrene infections at 4.3%, unknown sources of infection at 4.3%, and skin and soft tissue infections at 1.4%. These results are not much different from previous studies with lung infections (31%) and abdominal infections (26.3%) as the 2 (two) main sources of infection causing sepsis in ICU [16].
Characteristics of antibiotics used in the ICU
Based on the type of therapy, the antibiotics used in the ICU at Fatmawati Hospital are empirical and definitive therapy. The most use of antibiotics is as empirical therapy (64.1%) and definitive (35.9%). The most widely used antibiotic as empiric and definitive therapy is meropenem. The high empirical use of antibiotics in patients with sepsis and septic shock is due to the fact that patients with these conditions require immediate treatment, one of which is the administration of antibiotic therapy. The high mortality rate in patients with sepsis (20%) and septic shock (60-80%) requires early diagnosis and treatment. Antibiotics are given empirically until the determination of the active microorganism from the culture results is obtained [17]. The most widely used antibiotics in the intensive care unit are meropenem (33.8%), levofloxacin (13.6%), amikacin (12.3%), metronidazole (8.3%), ceftriaxone (7.9%), and amoxicillin-clavulanate (6.1%), as depicted in Figure 2.
Qualitative evaluation with the Gyssens method
The results of the evaluation of antibiotics based on the Gyssens category showed that most of the antibiotics were classified as rational (category 0) at 85.1% and irrational categories (categories I-V) at 14.9% (Figures 3 and 4). The accuracy of using antibiotics is quite high in the ICU ward of Fatmawati Hospital because the DPJP doctor is directly involved in monitoring the patient's progress. The PPRA program which has been running well, the existence of Guidelines for the Use of Antibiotics and Bacterial Maps as well as sensitivity to antibiotics at Fatmawati General Hospital are also one of the factors for the high accuracy of using antibiotics in the ICU ward. Most of the evaluated inappropriate use of antibiotics was included in category IV, which was 13.1% (Figures 3 and Table 1).

Figure 2: Percentage of use of antibiotics based on the prescription regimen given
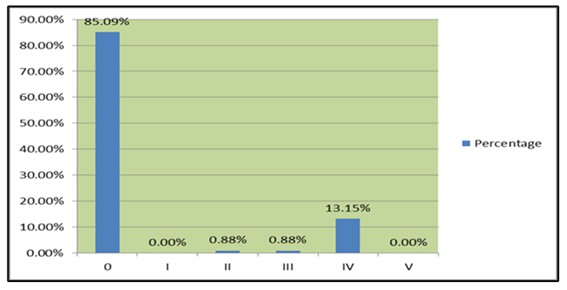
Figure 3: Total Percentage of antibiotics by Gyssens category

Figure 4: Types of recommendations given to doctors
Pharmacist intervention
The results of the evaluation of irrational antibiotics (category I-V) were 34 regimens, where from these results intervention was carried out in the form of giving recommendations to doctors as many as 34 recommendations.
Most recommendations were made on the problem of replacing antibiotics 31 recommendations (91.2%), suggesting duration of administration 1 recommendation (2.9%), changing the dose 1 recommendation (2.9%), and suggesting route of administration 1 recommendation (2.9%) (Figure 4).
According to the doctor's responses to the recommendations given, 64.7% (22 recommendations) were accepted and 35.3% (12 recommendations) were rejected (Figure 5). This is not much different from the Elkassas study which stated that of 104 recommendations regarding antibiotics made by pharmacists in the ICU, 68% were accepted by medical staff [18, 19]. Support from hospital management which provides flexibility and authority to clinical pharmacists in the ICU to evaluate the use of antibiotics is one of the factors that influence this. Good cooperation and communication between health workers is also one of the factors in the evaluating process of the use of antibiotics in the ICU [20-23].
Table 1: Distribution of antibiotic use based on Gyssens categories

Table 2: Specific recommendations made to prescribers

Evaluation with the Gyssens method was carried out again on antibiotics after giving recommendations, the results obtained for category 0 (rational) increased to 64.7%, category II decreased from 5.9% to 2.9%, category III decreased from 5.9% to 0% and category IV decreased from 88.2% to 32.4% (Table 3). Based on these results it can be seen that giving recommendations by pharmacists to doctors has increased the quality of rational use of antibiotics and reduced irrational use of antibiotics. The above results are in accordance with a cohort study that pharmacist intervention can increase the proportion of accuracy in selecting antibiotics in septic patients in the ICU from 66% to 80% [24].
Therapy outcomes
Assessment of treatment outcome was performed for all evaluated antibiotics (Figure 5). The total number of all antibiotic regimens evaluated was 228 regimens with 216 regimens included in category 0 (rational) and 12 regimens included in the irrational category.
Table 3: The results of therapy outcomes are based on the quality of antibiotic use


Figure 5: Results of evaluating the use of antibiotics with the Gyssens method before and after giving recommendations

Figure 6: Results of calculating the percentage of antibiotic use using the ATC/DDD method
Rational use of antibiotics has a mortality rate of 50% while irrational use of antibiotics has a mortality rate of 83.3%. Rational use of antibiotics, both qualitatively and quantitatively, will improve patient outcomes. According to this table, it can be seen that the quality of rational use of antibiotics has a mortality rate of 50%, which is lower than the quality of irrational use of antibiotics of 83.3%. These results are not much different from studies that state that irrational antibiotic prescribing causes mortality of 83% with a higher incidence of death observed in patients on ventilators, patients with serious drug interactions, and patients prescribed antibiotics irrationally [25].
Quantitative evaluation using the ATC/DDD method
The number of days of hospitalization for sepsis patients during August - November 2018 was 2731 days. The top five highest use of antibiotics in the ICU were meropenem 51.5%, levofloxacin 12.2%, amikacin 9%, metronidazole 9%, and ceftriaxone 4.6% (Figure 6 and Table 4). From the calculation results, it was found that the most antibiotic used was meropenem with a value of 32.9 DDD/100 patient-days, meaning that it is estimated that out of 100 sepsis patients in the ICU, 32 patients received 3 grams of meropenem per day (Figure 6).
A large DDD value indicates that the greater the level of use or quantity of antibiotic use, the greater the need for caution because it has a large potential for antibiotic resistance.
The high use of meropenem in the ICU ward at Fatmawati Hospital is possible because meropenem is included in the list of antibiotics recommended as empiric therapy for septic conditions and septic shock which has a broad spectrum of activity against gram-positive and gram-negative bacteria. Meropenem is a synthetic β-lactam antibiotic and is effective as an antipseudomonal its use is limited to patients with suspected infections caused by bacteria that are resistant to penicillin or cephalosporin groups which usually occur in patients treated in the ICU [26].
Characteristics of antibiotics used in the ICU
According to Figure 2, the graph is consistent with research that states that empirical antimicrobial therapy for sepsis and septic shock should have a broad spectrum from the start to maximize the range of potential microorganisms that are considered responsible for the underlying infection [5].
Based on the Guidelines for Antibiotic Use at Fatmawati Hospital, meropenem, levofloxacin, amikacin, metronidazole, ceftriaxone, and amoxicillin-clavulanate are antibiotics that are recommended to be used as empiric therapy in conditions of sepsis and septic shock [7, 27].
Qualitative evaluation with the Gyssens method
Most of the evaluated inappropriate use of antibiotics was included in category IV, which was 13.1% (Table 1). The problem that was found was the treatment that was not in accordance with the culture results. Even though the culture results showed resistance or intermediate, the use of antibiotics was continued. This can happen because the patient is almost resistant to all antibiotics available in the ICU, so the doctor decides to use the antibiotic with the lowest resistance.
The lack of supplies of several antibiotics is also one of the reasons for the inappropriate use of these antibiotics. The next most common problem is giving antibiotics that are too short and too long (category III), where antibiotics are only given for 1 (one) day, and then antibiotics are replaced. Empirical administration of antibiotics should be evaluated after 2-3 days of initial administration. The clinical condition of the patient becomes the doctor's consideration in replacing the antibiotic.
Therefore, it is necessary to have a good understanding of information about the spectrum of germs that cause infection and the pattern of sensitivity of germs to antibiotics.
Problems with the route of administration are the next factor that causes the inappropriate use of antibiotics. Certain antibiotics are given via the oral route (colistin), this is done because there is no supply of antibiotics in parenteral form, while based on the results of colistin culture, this is the only antibiotic that is still sensitive. Intravenous antibiotics should be started within the first hour after the patient is diagnosed with sepsis, every 1 hour of delayed administration of antibiotics will reduce survival by 7.6% [18].
Problems in determining the dose are the next factor that causes the inaccuracy of the use of antibiotics. In general, doctors have adjusted the dosage of antibiotics according to the patient's weight and kidney function, but there was still one case of inaccurate dosage.
Table 4: Calculation of the quantity of antibiotic use using the ATC/DDD method

In certain types of antibiotics, the patient's kidney function can determine the amount of antibiotic dose given, namely adjusting the dose according to the value of the patient's creatinine clearance test results [28, 29].
Factors that affect the quality of use of antibiotics
The Chi-square test was conducted to determine whether each variable type of antibiotic, type of therapy, number of drugs used by the patient, number of antibiotics used by the patient, doctor, and length of stay partially had a relationship to the variable quality of antibiotic use. The results of the Chi-square test obtained a p-value <0.05 indicating that the type of antibiotic, type of therapy, number of drugs, number of antibiotics, and length of stay are related to the quality of antibiotic use [30,31].
Differences in the quality of use of antibiotics before and after giving recommendations
The Wilcoxon test was carried out to determine differences in the quality of antibiotic use before and after giving recommendations. The hypothesis proposed is: that there is a difference in the quality of antibiotic use before and after the recommendation. In the calculation results, the calculated z value is -4,455 while the z table value is -1,645, with α = 5% and the calculated z value > z table (-4,455 > -1,645), then H0 is rejected which means there is a difference in the quality of antibiotic use between before and after giving recommendations.
Differences in therapeutic outcomes from several groups of quality antibiotic use
The Mann-Whitney test was conducted to determine whether there is an influence between the quality of rational use of antibiotics and the quality of irrational use of antibiotics on the therapeutic outcome. The calculation results obtained p= 0.025 (p <0.05) so that it can be stated that there is a difference in the therapeutic outcome between the quality of rational use of antibiotics and irrational use of antibiotics [32].
Conclusion
Factors that influence the quality of antibiotic use in sepsis patients in the ICU at Fatmawati Hospital are the type of antibiotic, the type of antibiotic therapy [33,34], the number of antibiotics, and the duration of antibiotic use [35]. Pharmacist recommendations can improve the quality of using antibiotics in the ICU ward of Fatmawati Hospital. There are differences in the therapeutic results between the quality of rational use of antibiotics and the quality of irrational use of antibiotics in the ICU ward of Fatmawati Hospital.
Acknowledgments
This study was supported and discussed with the teaching staff of the master of pharmacy study program at the University of Indonesia, Depok, Indonesia. We express our gratitude and appreciation to the University of Indonesia, Depok, Indonesia.
Disclosure Statement
No potential conflict of interest was reported by the authors.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors' Contributions
All authors contributed to data analysis, drafting, and revising of the paper and agreed to be responsible for all the aspects of this work.
The limitation of the research
The limitation of this research is that the recommendations or interventions carried out were not conveyed directly by the researcher to the prescribing doctor, but rather the recommendations were conveyed first to the pharmacist in charge of the ICU who will convey them back either orally or in writing on the patient's medication record sheet.
ORCID
Arief Fatkhur Rohman
https://orcid.org/0009-0009-5142-0762
Maksum Radji
https://orcid.org/0000-0002-3575-0704
Alfina Rianti
https://orcid.org/0009-0005-2141-686X
Arif Rachman
https://orcid.org/0009-0009-7069-1138
HOW TO CITE THIS ARTICLE
Arief Fatkhur Rohman, Maksum Radji, Alfina Rianti, Arif Rachman*, Evaluation of the Use of Antibiotics on Therapy Results of Sepsis Patients in the Intensive Care Unit (ICU) of Fatmawati Hospital, Jakarta. J. Med. Chem. Sci., 2024, 7(1) 262-274.


