Document Type : Case Report
Authors
1 Department of Anesthesiology and Intensive Care, Faculty of Medicine, Universitas Indonesia, Dr. Cipto Mangunkusumo Hospital, Jakarta, Indonesia
2 Department of Anesthesiology and Intensive Care, Faculty of Medicine, Universitas Diponegoro, Dr. Kariadi Hospital, Semarang, Indonesia
Abstract
Introduction: Quick and smooth recovery after bariatric surgery for morbidly obese patients may pose a challenge to anesthesiologists, especially if there is any cardiac comorbidity. The addition of spinal anesthesia besides general anesthesia is a strategy that can be considered in this procedure.
Case description: The 27 y.o. woman with a BMI of 53,8 kg/m2, atrial septal defect, and arrhythmogenic right ventricular dysplasia planned for bariatric surgery. The patient received preoxygenation for 24 hours before the day of surgery. After standard bedside monitoring for surgery had been applied, spinal anesthesia was administered at lumbal level L1–L2. General anesthesia was conducted after confirmation of a successful neuraxial block. Modifications of the surgical technique include low-flow CO2 insufflation. An episode of hypotension occurred once during the procedure and has been treated successfully with a 10 mg ephedrine bolus. Ventricle extrasystole appeared several times, but resolved with increasing oxygen fraction. Before extubation, infiltration of bupivacaine was done on a surgical wound. Paracetamol was intravenously administered for analgesia post-surgery. The patient was content with the anesthesia management and returned home without any complications.
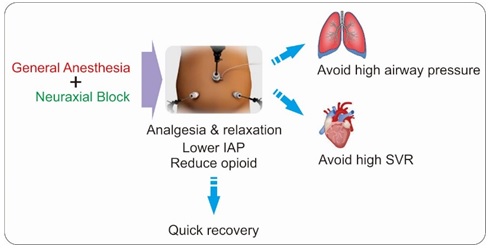
Discussion: A combination of anesthetic modalities may provide good abdominal relaxation, reduce the intraabdominal pressure during pneumoperitoneum, and reduce the use of muscle relaxants and opioids, which is important to gain optimal results in morbidly obese patients.
Conclusions: General anesthesia is widely used for laparoscopic bariatric surgery. The addition of spinal anesthesia in morbidly obese simple left-to-right atrial septal defect patients is still safe and may be a good alternative technique in selected cases.
Graphical Abstract
Keywords
Introduction
Obesity is a serious health problem that affects all organ systems. Obesity is defined as a disorder of lipid metabolism, characterized by excessive accumulation of fat in adipose tissue [1]. This has many health consequences, including increased risk of diabetes, obstructive sleep apnea, hypertension, dyslipidemia, coronary artery disease, gallbladder disease, osteoarthritis, osteoporosis, and socioeconomic and psychosocial disorders [2, 3]. One of the safe and effective methods for weight loss is bariatric surgery. This method is indicated in the presence of obesity when conservative treatments are ineffective [4, 5].
General anesthesia using volatile anesthetics and neuromuscular blockers is an anesthesia technique that is widely used for bariatric surgery [6]. Morbid obese patients often experience postoperative pulmonary complications after laparoscopic bariatric surgery, as general anesthesia can lead to increased intrapulmonary shunts and atelectasis [7, 8]. Patients with regional anesthesia experienced fewer pulmonary complications when compared with those who received general anesthesia [9]. However, certain side effects, such as more severe hypotension, shoulder discomfort, and requiring a higher sensory level, may come with regional anesthesia due to the diaphragma irritation, and breathing problems caused by pneumoperitoneum [10]. Combining these two techniques is expected to reduce the disadvantages of each technique and obtain advantages from both.
Laparoscopic sleeve gastrectomy (LSG) is one of the newer options in bariatric surgery. This method provides good results and can be done with a shorter duration [11]. Laparoscopic surgery has its advantages, but it should be noted that like any other surgical method, laparoscopy also carries a potential risk of complications [12]. During abdominal insufflation in laparoscopic, the distended abdomen caused by carbon dioxide insufflation can cause critical hemodynamic alteration and ventilatory change such as increased intra-abdominal pressure and hypercapnia. Increased intra-abdominal pressure further causes hemodynamic deterioration, and then increased afterload and reduced preload will decrease cardiac output, while ventilatory changes include increased peak airway pressure, hypercarbia, and decreased lung compliance. Patients with cardiovascular diseases such as ischemic heart disease, congestive heart failure, valvular heart disease, pulmonary hypertension, and congenital heart disease are more susceptible to catastrophic hemodynamic alteration during pneumoperitoneum [13].

Figure 1: Left to right shunt in secundum atrial septal defect based on Cardiac MRI
The atrial septal defect can lead to several consequences such as pulmonary hypertension, arrhythmias, and thromboembolic events. Anesthesia management in morbidly obese with congenital heart disease is a complex challenge. We reported successful anesthesia management in a case of bariatric surgery in a morbidly obese patient with atrial septal defect and arrhythmogenic right ventricular dysplasia.
Case description
A 27 y.o. woman with 121.4 kg bodyweight, 150 cm height, and a BMI of 53.8 kg/m2 is scheduled for bariatric surgery. Preoperative history reveals continuous weight gain and frequent nighttime awakenings due to the sudden shortness of breath. prior anesthesia exposures: one for a cesarean section with regional anesthesia and another for sedation during a gastroduodenoscopy, both without complications. Echocardiography results show arrhythmogenic right ventricular dysplasia (ARVD) and a secundum atrial septal defect (ASD) with a left-to-right shunt. Cardiac MRI with contrast also shows a secundum ASD measuring approximately 3 mm )Figure 1(, with a jet extending from the left to the right atrium.In addition, focal transmural delayed enhancement is observed at the mid anterior free wall of the right ventricle (RV), along with the mild reduction in RV ejection fraction (approximately 40.99%) and concentric thickening of the left ventricular (LV) wall.
Twenty-four hours before the surgery, the patient is administered oxygen at 3 lpm via a nasal cannula. In the operating room, routine monitoring includes ECG, oxygen saturation, and a noninvasive blood pressure cuff. A neuraxial block with spinal anesthesia is performed before the induction of general anesthesia. A low-dose injection of bupivacaine (7.5 mg) is administered in the subarachnoid space at the lumbar 1 and 2 levels. Block confirmation is achieved through pinprick testing and Bromage scoring. Once paresthesia is achieved at a supraumbilical level, and the Bromage score is zero, and then the patient is positioned in the RAMP position.
Preoxygenation with 6 lpm of 100% oxygen is carried out for 5 minutes before induction until FiO2 reaches 80-90%. Anesthesia induction is achieved using propofol 2 mg.kgbw-1, fentanyl 1 mcg.kgbw-1, and rocuronium 0.6 mg.kgbw-1 based on lean body weight, with endotracheal intubation facilitated using video laryngoscopy. Capnography is initiated after intubation. Laparoscopic sleeve gastrectomy is then performed, with insufflation of the abdomen using low-flow-rate carbon dioxide gas. Intra-abdominal pressure during insufflation ranges from 10 to 12 mmHg (Figure 2).

Figure 2: Laparoscopic sleeve gastrectomy can be done under low intraabdominal pressure (10-12 mmHg)
During the surgery, there is one episode of hypotension, which is successfully treated with 10 mg ephedrine administration. The surgery lasts for 2 hours. Furthermore, several instances of ventricular extrasystole improve with an increase in the inspiratory fraction of oxygen on the anesthesia machine ventilator. End-tidal CO2 on capnography is maintained between 30-35 mmHg. Maintenance anesthesia using sevoflurane and compressed air. There is no additional muscle relaxant or opioid administered until the surgery completion. Postoperative analgesia is provided by injecting bupivacaine and intravenous paracetamol around the surgical incision site. Extubation was performed in the operating theatre, and then monitored in the intensive care unit for a day before being transferred to a regular ward.
Patients with congenital heart disease are vulnerable to hemodynamic changes due to anesthesia and surgery. During laparoscopy, abdominal insufflation can cause a decrease in venous return, hypercarbia, and increased airway pressures. Other changes that occurred include increased pulmonary vascular resistance and reduced pulmonary blood flow [14]. High intraabdominal pressure can further burden the heart.
Insertion of the insufflation needle or trochar is the initial step for laparoscopic surgery, followed by insufflation of peritoneum space with by carbon dioxide (CO2) until intraabdominal pressure (IAP) reaches 12 to 15 mm Hg [15]. Increased IAP and hypercarbia are two main occasion of CO2 insufflation, that impact the cardiorespiratory and renal systems. Aortic compression, inferior vena cava compression, decreased splanchnic and renal blood flow, and diaphragmatic upward displacement are consequences of elevated IAP [16]. Inferior vena cava compression leads to complex venous return and resistance changes [17]. Pneumoperitoneum increases mean arterial pressure (MAP) and systemic vascular resistance (SVR) the final result is decreased cardiac output (CO) [18]. Diaphragmatic upward displacement can increase intrathoracic and airway pressure which can lead to ineffective respiration and reduce carbon dioxide elimination.
Many ASD patients have no obvious symptoms, although most will become symptomatic at some point in their lives. The age of onset of symptoms varies widely and is not solely related to the size of the shunt. Excessive pulmonary blood flow over a long period can cause pulmonary overflow, pulmonary hypertension, and right heart failure. Right atrial dilatation and stretch will give a clinical appearance as arrhythmias, especially atrial fibrillation or flutter [19]. Sympathetic increases such as hypoxia, hypercarbia, and pain, will cause further right heart burden.
In this case, a combination of general anesthesia and subarachnoid block was chosen with the hope that abdominal muscle tone would be more relaxed, thus keeping the increase in intraabdominal pressure relatively low. This was evidenced by intraabdominal pressures during pneumoperitoneum ranging from 10-12 mmHg. Spinal anesthesia provides uniform muscle relaxation, allowing the surgeon to perform laparoscopic procedures with lower intraabdominal pressure, typically 8-10 mm Hg, in non-obese patients [20]. The level of muscle relaxation achieved with spinal anesthesia cannot be attained in general anesthesia, even with the use of relaxant drugs, without undesirable depression of respiratory and circulatory functions [21].
Spinal anesthesia also gives good analgesia, reduces the need for muscle relaxants, and minimizes opioid requirements. Therefore, in obese patients, this strategy is advantageous as it allows for immediate spontaneous breathing and early extubation reducing postoperative pulmonary complications. Minimal opioid use preserves gastrointestinal peristalsis, preventing postoperative ileus. When used as an adjunct to general anesthesia, spinal anesthesia reduces postoperative pain and opioid consumption after laparoscopic procedures [22]. In this case, postoperative analgesia is effectively managed with intravenous paracetamol and peri-incisional bupivacaine infiltration.
The spinal anesthesia dosage is modified using a low dose of bupivacaine to ensure patient tolerance, especially in cases like this with an atrial septal defect. Low-dose bupivacaine (7.5 mg) has been reported as safe for patients with ASD and pulmonary hypertension undergoing non-cardiac surgery [23, 24]. With low-dose bupivacaine, peripheral vascular resistance does not decrease drastically, which can help reduce the workload on the heart. Perioperative changes in systemic vascular resistance (SVR) can have significant implications in patients with ASD [25]. In this case, there was one episode of hypotension that was successfully treated with ephedrine.
Despite several advantages of spinal anesthesia in this patient, morbid obesity poses a complication for spinal anesthesia. The patient's large abdomen makes it challenging to position for regional anesthesia. In this case, the patient was asked to sit with their legs hanging off the side of the operating table to facilitate the anesthesiologist during spinal needle insertion. Pre-procedural ultrasound-guided neuraxial anesthesia can help identify landmarks for neuraxial puncture and increase successful attempts.
Another comorbidity in this case is arrhythmogenic right ventricular dysplasia (ARVD). ARVD is a rare type of cardiomyopathy characterized by right ventricular dysfunction and ventricular arrhythmias [26]. It was diagnosed based on echocardiography and cardiac MRI findings in this case. ARVD pathology involves the diffuse or segmental loss of right ventricular myocytes by replacing fibrofatty tissue and thinning the right ventricular wall. The clinical spectrum of ARVD can range from asymptomatic presentation detected during family screening to sudden cardiac death.
Perioperative optimization plays a crucial role in ARVD cases, and one measure that can be taken is perioperative preoxygenation. This is especially important in morbidly obese patients who have a low functional residual capacity, as they are prone to rapid desaturation, which can accelerate cardiac dysfunction. Propofol is suitable for the induction and maintenance of anesthesia in patients with ARVD. Rocuronium has virtually no cardiovascular side effects and can be safely used in patients with ARVD [27]. If regional anesthesia is used, avoiding large doses of bupivacaine is advisable to reduce the risk of potential cardiac toxicity. Careful selection of opioid analgesia is recommended, with fentanyl considered as a safe option [28].
Conclusion
The advantages of combining spinal and general anesthesia in laparoscopic surgery are significant, especially for patients with congenital heart disease undergoing bariatric surgery.
Conflict of Interest
The authors reported no potential conflict of interest in this article.
Funding
This research received no specific grant from public, commercial, or not-for-profit funding agencies.
Authors’ Contributions
All authors contributed to data analysis, drafting, and revising of the article and agreed to be responsible for all aspects of this work.
ORCID
Bondan Irtani Cahyadi
https://orcid.org/0000-0003-3797-5779
Anas Alatas
https://orcid.org/0000-0002-7034-3645
Widya Istanto Nurcahyo
https://orcid.org/0000-0001-7534-0905
HOW TO CITE THIS ARTICLE
Bondan Irtani Cahyadi*, Anas Alatas, Widya Istanto Nurcahyo, Bariatric Surgery in Patient with Atrial Septal Defect and Arrhythmogenic Right Ventricular Dysplasia: an Anesthetic Challenge. J. Med. Chem. Sci., 2024, 7(1) 234-241.