Document Type : Original Article
Authors
1 Doctoral Program in Medical Science, Faculty of Medicine, Universitas Brawijaya, Malang, Indonesia, Department of Surgery, Division of Pediatric Surgery, Persahabatan General Hospital, Jakarta
2 Department of Clinical Pathology, Faculty of Medicine, Brawijaya University, Malang, Indonesia
3 Department of Nutrition, Faculty of Health Science, Brawijaya University, Malang, Indonesia
4 Department of Pharmacology, Faculty of Medicine, Universitas Brawijaya, Malang, Indonesia
Abstract
Background and objectives: Ulcerative colitis (UC) is an inflammatory disease of the large intestine characterized by diffuse mucosal damage accompanied by ulceration. UC is associated with proinflammatory cytokines. Currently, many herbal medicines are used to prevent various diseases. One of them, virgin coconut oil (VCO), is thought to be used as UC therapy.
Aims: To see the VCO supplementation effect as a prevention of Ulcerative Colitis by measuring inflammatory cytokine levels, Mouse Colitis Histopathology Index (MCHI) scores, and Disease Activity Index (DAI) scores.
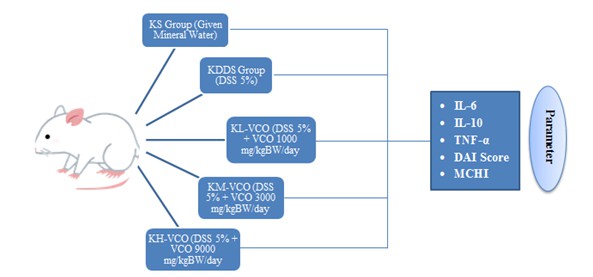
Materials and methods: This study used mice which were divided into 5 groups, namely the KS group (mineral water), the KDSS group (dextran sodium sulfate (DSS) 5%), the KL-VCO group (5% DSS + VCO 1000 mg/kgBW/day), the KM-VCO group (DSS 5% + VCO 3000 mg/kgBW/day), and the KH-VCO group (DSS 5% + VCO 9000 mg/kgBW/day). The treatment lasted 5 days, with observations of DAI score, MCHI score, and inflammatory cytokines (TNF-α, IL-6, and IL-10) were examined with an enzyme-linked immunosorbent assay (ELISA).
Results: When compared to the KDDS control group, the IL-10 levels of the treatment group that got VCO therapy went up as the doses of the KL-VCO group, the KM-VCO group, and the KH-VCO group went up in order. Besides, VCO therapy showed a decrease in IL-6 levels, TNF-α levels, DAI scores, and MCHI scores with increasing sequential doses in the KL-VCO group, the KM-VCO group, and the KH-VCO group when compared to the KDDS control group.
Conclusion: VCO supplementation can be used to prevent ulcerative colitis by increasing IL-10 levels while reducing IL-6, TNF-α, DAI, and MCHI scores. These effects can be caused by compounds in VCO with potential as anti-inflammatories and antioxidants.
Graphical Abstract
Keywords
Main Subjects
Introduction
Ulcerative Colitis (UC) is one type of Inflammatory Bowel Disease (IBD), a general term for diseases related to the immune system and inflammation of the gastrointestinal tract [1]. UC is an inflammatory disease of the large intestine that causes ulcers and mucosal demage. UC can cause stomach pain, diarrhea, bloody stools, anemia, and systemic symptoms like weight loss, anorexia, slow growth, delayed puberty, depression, and anxiety [2]. UC is clinically correlated with M1/M2 macrophages, TLR-4, and NF-kB activity. The mucosa of patients with UC is characterized by the accumulation of M1 macrophages that produce large amounts of inflammatory mediators through the NF-kB activation. Activated NF-kB is a heterodimer composed primarily of p65 and p50 units that can move from the cytosol to the nucleus to facilitate target gene transcription and induce the expression of proinflammatory genes such as TNF-α and IL-6 [3]. Glucocorticoids, immune complexes, and several cytokines (e.g., IL-4, IL-10, and IL-13) can induce polarization of M2 macrophages into different subclasses (M2a, M2b, M2c, and M2d). After IL-4 and IL-13 stimulation, M2a macrophages express CD206, high levels of IL-1 (IL-1R) and CCL17 receptors, and secrete profibrotic factors such as TGF-β, IGF, and fibronectin that are important for tissue repair [4]. Colon mucosal inflammation is one of the things that can be studied with UC model mice. The MCHI score (Mouse Colitis Histopathology Index) measures the severity, which looks at Goblet cell loss, crypt density, hyperplasia, and submucosal infiltration [5].
As for inflammatory therapy, currently many herbal medicines are used, one of which is virgin coconut oil (VCO). VCO is a processed product made from fresh coconuts whose oil is extracted by controlled heating or without any heating at all and processed without chemicals. VCO has nutritional and therapeutic benefits as an antioxidant, anti-inflammatory, antipyretic, and analgesic. VCO has bioactive components, including tocopherols, tocotrienols, and polyphenols, which may be responsible for the above effects.
Other ingredients are monolaurin, glycerol, and lauric acid, which are known to modulate inflammatory processes, have immunomodulatory and antimicrobial properties [6]. VCO Polyunsaturated Fatty Acid (PUFA) in the form of oleic acid, linoleic acid, and flavonoids functions as an anti-inflammatory. Linoleic acid has attracted the attention of food and supplement industries because it is a PPAR-g activator that is widely used as a diabetes therapy and has potential as an anti-inflammatory [7].
Several studies have been conducted to determine the effects of VCO as a supplement consumed daily or over an extended period of time. According to research, giving VCO helps lower cholesterol, control diabetes, and reduce obesity. High-density lipoprotein (HDL) levels can rise with VCO supplementation even over the long term in healthy people [8]. This demonstrates that long-term VCO use is generally harmless and can even treat physical problems and protect against disease. The study is unique because it uses native Indonesian VCO, whose benefits have not been studied much. Besides, not much research has been done regarding the relationship between VCO consumption and UC because VCO is well known as a dietary supplement for people with diabetes and high cholesterol. The study results are expected to provide a scientific basis for administering VCO to colitis in general to achieve a safe and efficient UC prevention composition with effective results, minimal complications, and relatively economical costs.
Martials and Methods
Materials
The VCO sample was created at the Palma Research Institute (Balit Palma), Ministry of Agriculture, Manado, Indonesia. BALB/c male rats weighing 20-24 grams and aged 6-8 weeks were used as animal models because they are more susceptible to develop UC than female mice [9]. About 30 mice were used, provided that each treatment group carried out five repetitions and the remaining one was used as a backup.
Methods
Mice were divided into five groups: (1) the negative control group (KS), given mineral water; (2) the positive control group (KDSS), given 5% dextran sodium sulfate (DSS); (3) the UC1 model group (KL-VCO), given 5% DSS + VCO at a dose of 1000 mg/kgBW/day; (4) the UC2 model group (KM-VCO), given 5% DSS + VCO at a dose of 3000 mg/kgBW/day; and (5) the UC3 model group (KH-VCO), given 5% DSS + VCO at a dose of 9000 mg/kgBW/day. The treatment of model animals is carried out according to the ethical standards stated in the ethical approval letter No. 256/EC/KEPK-S3/09/2021 from the Health Research Ethics Committee of the Faculty of Medicine Brawijaya University.
The mice were treated for 5 days. Clinical symptoms were observed using the Disease Activity Index (DAI), mucosal inflammation was assessed using the Mouse Colitis Histology Index (MCHI), and inflammatory cytokines (TNF-α, IL-6, and IL-10) were examined using the Enzyme-Linked Immunosorbent Assay (ELISA) as a parameter to assess colonic mucosal damage. In each group, 5 repetitions were carried out. If the data distribution was normal, One-way ANOVA was used, followed by post hoc LSD, and if the data distribution was not normal, Kruskal-Wallis was used, followed by Mann-Whitney. Results are considered significant if p <0.05.
Results and Discussion
The Effect of VCO on IL-6 Levels
Observations on IL-6 levels are displayed in Figure 1. Figure 1 demonstrates that the KDSS group had the highest level of IL-6 compared to the other groups. The KDSS group (72.58 ± 4.98) had significantly higher levels of IL-6 than the KS group (46.06 ± 12.30) (p = 0.000; p <0.05). Administration of 5% DDS showed an increase in IL-6 compared to KS. This shows that the administration of 5% DDS induces an inflammatory process that encourages ulceration of intestinal mucosa. The KL-VCO group (53.88 ± 17.17) was significantly higher than the KM-VCO group (35.42 ± 6.37) (p = 0.004; p <0.05) and KH-VCO group (24.53 ± 3.43) (p=0.000; p<0.05). IL-6 is one of the biomarkers showing how inflammation can affect the immune system. In this study, there was a significant decrease in IL-6 levels in the group that received higher doses of VCO compared to the control group. The results showed that with higher dose of given VCO, the expressed IL-6 level is decreased. The treatment group that received 1000 mg/kg/day VCO had significantly higher IL-6 levels than those that received 3000 mg/kg/day or 9000 mg/kg/day VCO. The lowest IL-6 levels were found in the KH-VCO group (9000 mg/kg/day).

Figure 1: Results indicate levels of IL-6

Figure 2: Results indicate levels of IL-10
This indicates that it is suspected that with higher dose of VCO, the effect on colonic mucosa repair is increased. The findings of this study are consistent with the findings of another study, which found that the VCO treatment group could decrease CRP, IL-6, and PG2 levels compared to the control group [10]. The study found that giving VCO to the treatment group resulted in a significant increase in anti-inflammation. VCO has an antiulcer and free radical activity similar to the omeprazole drug, namely an increase in GSH and nitrite levels corresponding to a decrease in MDA, CAT, SOD, and GP that appears with VCO. VCO significantly increases superoxide dismutase activity. Furthermore, compared to omeprazole-treated animals, there was an improvement in epithelial tissue and a decrease in cell number after VCO administration [11]. According to the other studies, increasing the dose of VCO reduces IL-6 levels. This can be explained by the composition of VCO, which is high in polyphenols, which have been shown to affect the inflammatory chain reaction, and thus prevent pathogenesis. Polyphenols fight inflammation through indirect mechanisms that release anti-inflammatory signaling molecules [12]. As a result, it can be concluded that VCO administration can reduce IL-6 levels. This is most likely due to the polyphenol-rich content of VCO, which affects the inflammatory response, and thus slows down the disease progression.
Effect of VCO on IL-10 levels
Observations on IL-10 levels are depicted in Figure 2. Figure 2 demonstrated that the IL-10 level in the KS group was significantly higher than the KDSS group (1.72 ± 0.52) (p = 0.000; p <0.05), KL-VCO (2.91 ± 1.15), and KM-VCO (5.93±0.74) (p=0.000; p<0.05). IL-10 levels in experimental animals increased significantly with increasing doses of given VCO (p<0.05). In the group with the highest dose (KH-VCO), IL-10 levels increased as high as the control group (p=0.474; p>0.05).
IL-10 inhibits the production of pro-inflammatory cytokines and chemokines by macrophages and dendritic cells activated by Toll-like receptor agonists (TLRs), LPS, and bacterial lipoproteins. Extensive genetic and pharmacological studies on animals have established that IL-10 plays an important role in limiting chronic and acute inflammation [13].
This study obtained the highest to lowest IL-10 levels, namely KS, KH-VCO, KM-VCO, KL-VCO, and KDSS. IL-10 levels in the KS group were significantly higher than in the KDSS and treatment groups. This demonstrates that at higher doses, VCO increases IL-10 levels. The findings of this study are consistent with the literature, which states that VCO is a modulator of the inflammatory cascade that prevents inflammation. In particular, polyphenols activate an indirect mechanism for releasing anti-inflammatory signalling molecules like IL-10 and reduce IL-1 β -induced DNA binding activity of NF-kB p65 to prevent inflammation [14]. According to other studies, VCO can increase IL-10 levels as an anti-inflammatory cytokine [15]. The results of this study show that VCO can increase IL-10 levels. This is likely because VCO can change the inflammatory cascade and stop inflammation from happening. VCO also contains polyphenolic compounds, which trigger the release of anti-inflammatory signalling molecules.
Effect of VCO on TNF-α levels
TNF- α levels were measured to examine the systemic inflammatory response, and the results are demonstrated in Figure 3. Figure 3 illustrates that 5% DSS administration significantly increased TNF-α levels compared to the control group (p = 0.00; p<0.05). TNF-α levels were decreased when the VCO dose was increased compared to the KDSS group (p<0.05). At the highest dose of VCO, it reduced TNF-α levels like the KS group (p=0.891; p>0.05). Tumor necrosis factor (TNF-α) is a pro-inflammatory cytokine responsible for inflammation, tissue damage, and cell death. TNF-α is widely studied as a pro-inflammatory cytokine that plays a key role in the pathogenesis of various inflammatory diseases [16]. The findings of this study on the systemic inflammatory response revealed that all groups given VCO had reduced TNF-α level. The TNF-α value was the lowest in the KH-VCO group, which received 9000 mg/kg/day. This demonstrates that VCO affects TNF- levels in an indirect manner. According to the literature, VCO administration can reduce TNF-α, iNOS, IL-1, COX-2, and IL-6 density values in lipopolysaccharide-induced RAW 264.7 cells [17]. Other studies concluded that the presence of phenols, flavonoids, and vitamin E in VCO, emphasizing its high antioxidant properties, as well as the presence of several fatty acid components, such as lauric acid, contributed to VCO's effective role in ulcer prevention. In conclusion, VCO exhibits potential mucosa-protective activity in various ulcer models. VCO is a potential therapy used to treat and prevent inflammation [16], so it can be concluded from this study that VCO was indirectly effective in reducing TNF- α levels.
Effect of VCO on disease activity index (DAI) score
In addition to observe the characteristics of inflammatory cytokines, the Disease Activity Index (DAI) score was calculated with the results shown in Figure 4. Figure 4 displayed that the disease activity index (DAI) score in the positive control and treatment groups increased daily. A significant increase was seen especially on the fifth day.

Figure 3: Results indicate levels of TNF-α

Figure 4: Results indicate of DAI score
The KDSS group had the highest average score of 7.33 ± 1.21 followed by KL-VCO, KM-VCO, and KH-VCO with respective values of 4.00 ± 2.53, 2.50±1.87, and 1.20±0.84.
In this study, VCO administration improved weight loss, faecal form, and faecal blood. The DAI score can be used to calculate this. A DAI score was used for the evaluation of severity of colonic inflammation in rats after 7 days of the treatment [19]. The administration of VCO to all treatment groups resulted in significantly lower results when compared to the KDSS group, and there was a significant difference in DAI scores in the KS group compared to all groups. Statistical tests showed that administering VCO can lower the DAI score. This demonstrates that VCO has been shown to improve clinical symptoms in UC mice. These findings are consistent with a study that found that agents with high antioxidant properties, such as VCO, can protect the mucosal layer from necrosis agents like ethanol. The mechanism is that VCO increases mucus secretion on the mucosal surface and contributes to ROS formation. VCO has further been reported to have strong anti-oxidant properties due to its flavonoid and fatty acid components [20]. Other research has shown that VCO has the most potent antiulcer activity. The ability of antiulcer activity is linked to Free Fatty Acid (FFA). FFA has been shown to have pharmacological effects such as antioxidants such as palmitic acid and myristic acid, as well as anti-inflammatory properties such as linoleic acid, oleic acid activity, and lauric acid [21]. It can be concluded that VCO administration can reduce the DAI score, which assesses weight loss, stool form, and stool blood. This is presumably because VCO can increase mucus secretion and play a role in reducing ROS. VCO also contains high levels of antioxidant properties due to flavonoids and other fatty acid components.
Effect of VCO on mouse colitis histology index (MCHI) score
The MCHI score was used to assess the degree of damage to the colonic mucosa after administration of 5% DSS and VCO. The graph of the MCHI score after the administration of DSS and VCO can be seen in Figure 5. Figure 5 demonstrates that the MCHI score in the KDSS and treatment groups is higher than in the KS groups. The KDSS group had the highest average score of 16.00 ± 8.10 followed by KL-VCO, KM-VCO, and KH-VCO with respective values of 15.58 ± 1.59, 12.42 ± 1.20, and 5.08 ± 4.08. In addition to the DAI score, an MCHI score was assessed to assess the degree of damage to the colonic mucosa after VCO administration. Mouse Colitis Histology Index (MCHI) was used to measure histopathological changes [22]. This study found that all treatment groups experienced a significant decrease compared to the KDSS group. The higher the VCO dose, the lower the MCHI score. This shows that administering VCO can repair damage to the colon mucosa with increasing doses. The results also align with the literature, which states that VCO can increase the proliferation of fibroblast cells so that the density of collagen fibers increases and wounds treated with VCO heal faster. This is evidenced by a decrease in complete epithelialization time and a higher re-epithelialization rate [23]. In other studies, coconut oil contains fatty acids with relatively short chain lengths, although this is not identical to short chain fatty acids (SCFA), which are defined in colitis therapy. VCO showed a positive impact on epithelial metabolism, as postulated for SCFA. VCO substantially reduced epithelial cell necrosis. One week after the initiation of daily coconut oil administration, the patient reported decreased abdominal pain and mucus secretion. After 6 weeks of continuous therapy, the hematochezia and mucous secretions have completely stopped. Within 8 weeks of therapy, there was a significant improvement in the signs of inflammation seen on endoscopic and histological examination.

Figure 5: Results indicate of MCHI score
After 12 weeks of treatment, the patient is pain-free, returns to work, and is physically active 3 to 4 times a week. After 5 months of endoscopy, only low-grade inflammation was found. Likewise, histological improvement was found. Patients have continued daily application of coconut oil for 6 months with continuous improvement in clinical response and no side effects [24]. VCO Polyunsaturated Fatty Acid (PUFA) acts as an anti-inflammatory in the form of oleic acid, linoleic acid, and flavonoids. Linoleic acid is a PPAR-(activator) widely used in diabetes therapy and has anti-inflammatory potential [7]. This supports the results of this study, indicating that the anti-inflammatory effect of VCO can repair damage to the colon mucosa, thereby reducing the MCHI score. VCO has been shown to increase anti-inflammatory cytokines such as IL-10 and reduce proinflammatory cytokines such as IL-6 and TNF-a. However, the cytokine mechanism changes due to VCO administration in this study still requires further research. According to the findings for each evaluated parameter, VCO's potential as an anti-inflammatory and antioxidant agent plays a role in the management of ulcerative colitis. This is demonstrated by its clinical impact on the inflammatory cytokine markers examined in this investigation. These inflammatory cytokines are linked to the ulcerative colitis prevention or improvement, which results in fewer symptoms.
Conclusion
According to the findings of this study, VCO administration can increase IL-10 levels while decreasing IL-6, TNF-α, DAI, and MCHI scores. These effects are based on the content of compounds in VCO that act as anti-inflammatories and antioxidants. For future research, it is necessary to complete the intermediate and confounding variables to obtain a comprehensive and thorough understanding of the effects of giving Indonesian native VCO to UC.
Conflict of interest
No potential conflict of interest was reported by the authors.
Disclosure Statement
No potential conflict of interest was reported by the authors.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors' Contributions
All authors contributed to data analysis, drafting, and revising of the article and agreed to be responsible for all the aspects of this work
ORCID
Ni Made Rika Trismayanti
https://orcid.org/0000-0002-4708-0170
Kusworini Handono
https://orcid.org/0000-0002-4899-2454
Dian Handayani
https://orcid.org/0000-0001-9018-0233
Umi Kalsum
https://orcid.org/0000-0002-9968-3627
HOW TO CITE THIS ARTICLE
Ni Made Rika Trismayanti*, Kusworini Handono, Dian Handayani, Umi Kalsum., Virgin Coconut Oil Supplementation as Ulcerative Colitis Prevention, Does it work? : Clinical Correlation. J. Med. Chem. Sci., 2023, 6(12) 3178-3187.