Document Type : Original Article
Authors
- Abdel Wahab Abdelsattar Saleh Mohammad 1
- Maher A sheriff 1
- Yara Ayman Iskandarani 1, 2
- Wael Mohammed Mossa 3
- Mohamrd Hamdi Alqassas 1
1 Anesthesia, ICU and Pain Management, Faculty of Medicine, Alazhar University, Cairo, Egypt
2 Intern Doctor, Department of Medicine, Bahçeşehir University, Istanbul, Turkey
3 Anesthesia Specialist, Fakeeh University Hospital, Dubai, United Arab Emirates
Abstract
Background: Endotracheal intubation is a routine procedure in the ICU that may save a patient's life. The stridor probability after extubation increases with a smaller cuff-leak volume. This research aimed to estimate the efficiency of the cuff leak test vs. laryngeal U/S in identifying post-extubation stridor in prone surgical patients under general anesthesia.
Methods: Seventy-five adults with ASA status I or II who would be undergoing prone, general anesthetic, and elective spine surgery took part in this prospective cohort research. All patients underwent a complete medical history, physical examination, laboratory tests, and laryngeal ultrasonography. Cases were examined for post-extubation syndrome (PES) and the necessity for reintubation.
Results: PES occurred only in 15 (20%) patients. Cut-off pressure, CLT for PES, and air column width before deflation were insignificantly different between the entire population and the PES group. ACWD was a significant predictor of PES incidence at a cut-off value of 0.8 mm, AUC = 0.715, and P = 0.02 with 71.43% sensitivity, 78.33% specificity, 43.5% PPV, and 92.2% NPV. CLT was an insignificant predictor of PES incidence.
Conclusions: The US measurement of ACWD is a reliable method of forecasting PES.
Graphical Abstract
Keywords
Main Subjects
Introduction
Endotracheal intubation is frequently utilized in intensive care units since it improves survival rates [1]. Patient placement is essential for patient safety and an optimal surgical outcome. Patients are less likely to have complications after surgery when they are in the correct position [2, 3]. The prone position is necessary for the majority of neurosurgical, urological, general, and spinal surgical procedures [4].
Fewer options exist for head and neck repositioning during bag-mask ventilation (BMV) when the patient is prone, airway access is restricted, and the endotracheal tube (ETT) may migrate (during head extension and flexion, the ETT tip moves cephalad or caudad) [5, 6].
Since the prone position offers the most favourable working conditions and operative-site exposure, it is often employed for multilevel cervical, thoracic, and lumbar spine surgeries [7]. Due to the potential for significant tissue edema in prone patients, careful planning for extubation after surgery is required [8]. To prevent airway edema, authors suggest restricting crystalloid administration [9]. This is because various organs can keep functioning properly thanks to the vasopressors injection. It is unclear from the available research whether or not fluid infusion in the prone posture causes airway edema and consequent breathing problems [8].
Edema, ulceration, granulation, and immobility of the vocal cords are frequent outcomes of laryngeal trauma during endotracheal intubation [10]. Laryngeal edema (LE) is a common obstacle that arises after intubation and is the result of the endotracheal tube's direct pressure and the inflammatory response on the contact surfaces. The pathological process leading to edema begins immediately after intubation, although the clinical presentation of it does not arise until the endotracheal tube is removed [11].
Factors associated with pulmonary embolism (LE) in intubated patients have been investigated [12]. Previous research has shown that tracheoesophageal fistula is more likely to occur in women, when intubation is difficult, when patients self-extubate, and when intubation procedures take too long. Both Chung et al. [13] and de Bast et al. [14] were unable to pinpoint a single cause of LE and/or stridor in their studies.
It is crucial to diagnose and treat post-intubation laryngeal edema prior to extubation since reintubation may increase morbidity and mortality [15].
Low cuff-leak volume increases the PES likelihood. The cuff-leak test (CLT) was discussed by Miller and Cole [16] as a possible indicator of clinically severe laryngotracheal constriction. The patient's upper airway patency may be evaluated by cricothoracic (CLT) surgery by deflating the balloon sleeve of the ETT. PES is more prevalent in those with smaller cuff leakages. The degree of cuff leak varies across trials, leading surgeons to make difficult choices about extubation based on a favourable CLT [17, 18].
Ultrasound imaging is a unique, simple, lightweight, and non-invasive instrument for evaluation and treatment of the airway in the operating theatre, emergency room and ICU. In the medical era, ultrasound imaging of the upper airway is used for different purposes, such as locating the ETT, guiding a percutaneous tracheostomy or cricothyroidotomy, diagnosing subglottic stenosis, determining the likelihood of difficult intubation or PES, and determining the appropriate size of an ETT for a child [19, 20].
Air Column Width (ACW), or acoustic shadow breadth at the cords' level in cases who have been intubated, is determined both prior to and following cuff deflation. It is possible that this method may accurately forecast the chance that stridor will occur following extubation. The ACWD is calculated by comparing the intubated and deflated air column measurements [21].
We aimed to compare the CLT and laryngeal U/S for the detection of PES in patients who underwent surgical procedures in prone position with general anesthesia.
Materials and Methods
The prospective cohort research was done on 75 American Society of Anaesthesiologists (ASA) Status I or II participants who were supposed to have elective spinal operations in the prone position under general anesthesia. Cases gave their informed permission in writing. Following sanction from the Faculty of Medicine's Ethical Committee, the investigation took place.
Cases with expected harder airways (Mallampati Grade III and IV, or thyromental distance <6 cm and/or restricted mouth opening) intubation following greater than 2 attempts, with expected or real need for blood transfusion, with cardiac or pulmonary illnesses, who were long-lasting smokers, had upper airway infection within the previous 2-3 weeks, and with expected requirements for mechanical ventilation (MV) after surgery were eliminated from the research.
Cases were not administered any premedication. To elicit anesthesia, propofol 1-2 mg/kg and fentanyl 1.5 μg/kg were administered, and then for easier orotracheal intubation with a cuffed armored tube, rocuronium 0.6 mg/kg was given. Male cases were intubated with a tracheal tube of size 7.5, while female cases were intubated with a tracheal tube of size 7.0, and tracheal cuff was inflated to twenty-five cmH2O. To achieve an end-tidal CO2 concentration of about 35 mmHg, the volume-controlled MV was modified.
Monitoring was performed using pulse oximetry, end-tidal CO2, electrocardiography, invasive and non-invasive blood pressure, oesophageal temperature, urine output through a Foley catheter, and blood loss. Anesthesia was kept up with sevoflurane, rocuronium, and fentanyl infusions and oxygen in the air (50:50).
Five minutes after intubation, while patients remained supine, the spirometer on the anesthesia machine recorded the inspired tidal volume (VTi) for three subsequent breaths. The tracheal ligature was then depressed completely, and the expired tidal volume (VTe) was measured for three successive breaths.
For analysis needs, the mean of three measurements (both inspiratory and expiratory) was determined. This period was designated as T1, and the breach volume (CLV) was determined as the distinction between VTi and VTe. Thereafter, the cases were positioned prone on a Jackson table with the neck either in a neutral or slightly bent posture.
Every case underwent a comprehensive history (age, gender, and BMI), clinical examination (heart rate, blood pressure, pulse, and temperature), and lab examination. After extubation, cases were examined for PES and necessary reintubation. The existence of an inspiratory wheeze so severe that it needs medical attention was defined as PES. PES was followed by a respiratory rate >30/min or a rise of >10/min from baseline [22]. PES has been linked to respiratory distress in 24 hours following extubation.
Cuff leak test (CLT)
When the case was thought to be prepared for extubation, the cuff loss was measured. The CLT was conducted immediately after intubation (T1) and prior to extubation (T2). Miller and Cole [16] suggested a protocol, which was followed during the procedure. Oral and endotracheal secretions were vacuumed, and the ventilators were set to assist-control mode prior to the test assessment. When the cuff was inflated and deflated, tidal volume (VT) was determined. The average value was determined after measuring six consecutive respiration cycles. CLV was derived from the distinction among VT prior to and following cuff deflation. Measuring the variation in CLV among T1 and T2 was used to assess airway edema.
Assessment and management of airway edema
Edema development in the larynx and hypopharynx in the prone position can result in airway blockage after extubation. Clinical indicators of upper airway edema as swollen neck veins, orbital, facial or conjunctival edema, and head venous congestion. Prior to tracheal extubation, it may be beneficial to check the extent of airway edema with a flexible nasopharyngoscopy, despite the absence of evidence confirming its clinical utility. There are no scientifically confirmed methods for evaluating the degree of airway edema or predicting post-extubation airway blockage. It has been suggested that prior to extubation, individuals with suspected airway edema should undergo a leak test [23].
In a patient who is mechanically ventilated, the leak test evaluates the difference between tidal volume before and after cuff deflation. When a sufficient leak is present, it remains unclear whether a test result is positive or negative. However, a greater cuff leak volume (> 88 - 140 mL or > 10 - 18 % of the pre-deflation expired or inspired volume) has been demonstrated to indicate adequate airway patency to sustain extubation without postextubation stridor (PES) [24].
The leak test can also be conducted by deflating and occluding the proximal end of the ETT in a patient who is spontaneously breathing without ventilator support. When there is evidence of an audible leak or coughing around the ETT, a positive leak test is confirmed. The absence of a leak and/or coughing is indicative of PES [25]. This test was judged beneficial for alerting the clinician of a high risk of upper airway blockage when the leak rate was lower that the predetermined threshold. Nonetheless, a leak that exceeds the predetermined level does not exclude PES.
Laryngeal Ultrasonography (US)
The laryngeal US was carried out using a Medisoneaccuvix-v10 probe liner (7/5 MHz) to image the vocal cords (VCs) in accordance with the protocol laid out by Ding and colleagues [26]. An expert radiologist (M.K.T.) conducted all US assessments. Cases were positioned supine with their necks hyperextended. The balloon closure was inflated and deflated during the test. The US demonstrated that the laryngeal ACW corresponds to the breadth of air passing through the VCs. It was documented three times in a row, and the average value was noted.
The VCs, the adjacent soft tissues, the air flowing through the VCs (the laryngeal ACW is regarded as the width of air passing through the VC as assessed by US), and the shape of the air column were observed.
The VCs, the adjacent soft tissues, the air flowing through the VCs (the laryngeal ACW is regarded as the width of air passing through the VC as assessed by US), and the shape of the air column were observed [17, 26]. The air-column variation was determined as the variation in width among balloon-cuff inflation and balloon-cuff deflation, whereas a shift in the air column was noted as the base of the air column widened with balloon-cuff deflation because of distortion when air flows among ETT and VC. The physician observed that the ACW difference (ACWD) was the width variation between balloon-cuff inflation and deflation between balloon-cuff deflation and balloon-cuff inflation during 3 breathing cycles, after the median values.
In a subset of cases, bronchoscopic images were obtained before extubation to enable immediate observation of the VCs with the ETT in position and to facilitate association among US and bronchoscopic images. When feasible, bronchoscopy was performed following extubation to evaluate changes in VC volume and movement, particularly in cases with stridor or those who needed reintubation [27, 28]. Stridor is defined as the development of a high-pitched inspiratory wheeze localized to the larynx or trachea and associated with respiratory distress, which usually required medical intervention.
Sample size calculation
Using G. power 3.1.9.2 (Universität Kiel, Germany), the sample size estimation was conducted. N ≥72 was determined as the sample size owing to the subsequent factors: 0.05 α error and 80 percent power of the investigation to determine the frequency of PES varied from 9 to 30 percent owing to previous research [29]. To combat dropout, 3 cases were introduced to each cohort. Accordingly, 75 cases were selected.
Statistical analysis
SPSS v26 (IBM Inc., Armonk, NY, USA) was used for statistical analysis. Quantitative variables were presented as means (± SD) and compared between the 2 groups by an unpaired Student's t- test. Qualitative variables were examined using the Chi-square or Fisher's exact test when appropriate and presented as frequency and percentage. ROC curve analysis was used to evaluate diagnostic performance by diagnostic sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV), as well as the overall diagnostic efficacy of each test. A two-tailed P value less than 0.05 was deemed to be substantial.
Results and Discussion
Baseline characteristics (age, sex, weight, height, and BMI) were inconsequentially different amongst the researched groups, as listed in Table 1.
The mean disease severity score was inconsequentially different among the researched groups (27.8 ± 7.39 in group I vs. 29.8 ± 7.13 in group II). Fusrthermore, the mean intubation period was inconsequentially different among the researched groups (56.6 ± 8.12 in group I vs. 56.0 ± 8.53 in group II), as presented in Table 2.
The mean air column width was insignificantly different between the examined groups (0.9 ± 0.09 in group I vs. 0.8 ± 0.17 in group II). The mean cut off pressure was insignificantly different between the examined groups (34.1 ± 8.87 cmH2O in group I vs. 35.6 ± 9.58 cmH2O in group II).

Moreover, the mean CLT was insignificantly different between the examined groups (335.67±168.06 in group I vs. 250 ± 146.15 in group II). Air column width and cut off pressure had no discernible effect on the examined groups, as provided in Table 3.
Cut off pressure was ≤25 cmH2O in 24 (32%) patients among the entire population and in 2 (13%) patients in PES group was >25 cmH2O in 51 (68%) patients among the entire population and 13 (87%) patients in PES group. CLT for PES was positive ≤249 mL in 29 (39%) patients among the entire population and in 4 (27%) patients in PES group and was negative (>249 mL) in 11 (61%) patients among the entire population and in 11 (73%) patients in PES group. Air column width before deflation was <10.95 mm in 45 (60%) patients among the entire population and in 6 (40%) patients in PES group and was >10.95 mm in 30 (40%) patients among the entire population and 9 (60%) patients in PES group. PES occurred only in 15 (20%) patients. Cut off pressure, CLT for PES and air column width before deflation were insignificantly different between the entire population and PES group, as presented in Table 4 and Figure 1.
ACWD was a significant predictor of PES incidence at cut off value ≤0.8 mm, AUC =0.715 and P=0.02 with 71.43% sensitivity, 78.33 % specificity, 43.5 % PPV, and 92.2 % NPV. CLT was an insignificant predictor of PES incidence, as indicated in Table 5 and Figure 2 and 3.

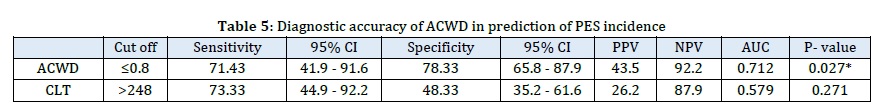
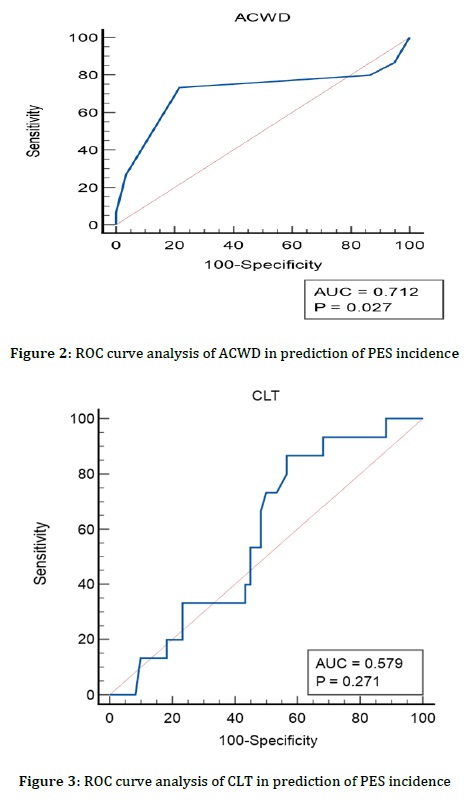
It is believed that airway edema results from transient venous congestion of the head and neck in conjunction with increased intraoperative fluid infusion during prone surgery [30]. Although all intubated cases experience laryngeal edema, it is typically temporary and self-limiting, and only a minority of cases develop clinical symptoms. In more extreme cases, edema can lead to PES, which can result in acute respiratory distress and necessitate critical re-intubation [31]. In addition to the prolonged intubation, factors such as great cuff pressure or great tube size in relation to laryngeal size, female gender, BMI >26.5 kg/m2, and previous intubation difficulties or self-extubation increase the likelihood of PES [32].
Excessive anteflexion of the neck in the prone position during surgery can also put the patient at risk for airway edema, which can make it hard for them to breathe after they are extubated [33].
The anatomic alterations in the airway may occur in cases in the prone position because of trauma related to airway management after induction of anesthesia, surgery (around the cervical spine), the prone position, or airway treatment for a dislodged ETT. Airway anatomy can be altered by cervical vertebral fixation and surgical alterations to the oropharyngeal and neck structure [34, 35].
Because of fluid resuscitation, extended surgical operations with substantial blood loss may be linked to airway edema. The dependent posture and direct pressure on the face and neck structures impede venous drainage and are linked to the formation of edema [8]. Airway edema can obscure the larynx and make it difficult to see its components. In addition, Edematous tissues may be more susceptible to trauma. All of these are crucial considerations prior to extubation at the conclusion of the procedure [36, 37].
Postextubation LE is believed to originate from direct mechanical stress to the larynx generated by the ETT and is a common reason for airway blockage following extubation in instances needing ICU [38]. Depending on the degree of airway obstruction caused by LE, emergency reintubation may be required [15, 39]. Reintubation is associated with a rise in MV days and duration of stay in the ICU, as well as an increase in costs, morbidity, and mortality [40].
Research on postintubation LE has been published. However, most of these have been conducted in ICUs, where cases are intubated for extended periods of time [41, 42].
To the best of our knowledge, there is a paucity of studies that detect post-extubation strider in patients who underwent a surgical procedure in a prone position with general anesthesia.
Jan et al. [8] discovered that Procedures that are done in the prone position are correlated with a wide range of difficulties that, if left untreated, can result in significant morbidity. From pressure injuries of the epidermis to the optic neuropathy, anaesthesiologists fear a wide range of potential dangers. Post-extubation airway edema is the primary cause of airway emergencies and unanticipated ICU admissions following surgery. Since airway edema can be potentially fatal, it is essential to study any factors contributing to its development.
The PES diagnosis is clinically essential because cases with this condition may profit from close monitoring and specific treatments. Nevertheless, there is not any agreement regarding a technique for identifying cases at hazard for PES. The CLT, which demonstrates a leak around the ETT with the cuff deflated, has been suggested as a straightforward technique to forecast PES incidence [15]. However, the termination point of the CLV varies significantly among previous investigations and the contradictory outcomes may force clinicians to make challenging extubation decisions. Consequently, there is an essential requirement for characterizing the hazards of PES development via alternative methodologies [43, 44].
The CLT was not a reliable indicator of the occurrence of PES. We observed that CLT was sensitive in predicting PES (73.33%). In addition, the low PPV values for CLT methodologies may indicate that they are unable to reliably evaluate PES.
The PES prediction cutoff factors for CLT are still the subject of debate. Miller and Cole demonstrated that a cuff loss volume of <110 mL may indicate a patient's susceptibility to PES [16]. Jaber et al. [45] discovered that cuff leak volume values <130 mL were linked to a higher probability of PES. Most of the research on CLV reported high specificity and NPV, indicating that cases with a CLV over a particular limit had a low likelihood of developing PES. Notwithstanding, the low sensitivity and PPV of these methodologies may be pointing to their restricted predictive value for PES. Taking into account their cutoff values are (<110 mL and <130 mL) [45, 46].
Ochoa et al. [24] aimed to assess diagnostic review and meta-analysis of studies assessing diagnostic precision of the CLT for upper airway blockage involving more than 50 patients. The combined specificity and sensitivity were 56 percent and 92 percent, respectively. It was established that this test was helpful since it warned the physician of a greater likelihood of upper airway blockage when the leak rate was below the set threshold. Nonetheless, a breach that exceeds the predetermined threshold does not always exclude PES.
A second comprehensive analysis found that the specificity was greater for cases who had been using an ETT for longer than 5 days [13]. Research has concluded that the CLT is either useful for predicting adverse events or is not useful, even though they all afflicted with several limitations in research strategy. Therefore, clinicians should be aware of restrictions of the CLT. Moreover, research was conducted on cases in ICUs and may not be pertinent for after surgery extubation in the operating room in prone cases [47, 48].
However, Mikaeili et al. [22] CLT 249 mL, a figure far larger than the recommended values in the prior trials, was shown to have good sensitivity and NPV but low PPV. On the other hand, Engoren et al. [49] found that in all 3 PES cases, CLT values were greater than 310 mL. The overall clinical decision to initiate PES therapy based only on CLT outcomes may be difficult.
Additional approaches are required to identify high-risk patients prior to extubation. One potential approach for predicting PES and laryngeal edema is laryngeal ultrasound (US) to assess the ACW before cuff deflation and ACWD [50, 51].
There is a lack of studies that assess the function of US in in forecasting PES in prone position using US ACWD was determined by noting the shape of the air column prior to and following deflation of the cuffs. Therefore, we conducted this research to contrast the CLT and laryngeal U/S for detection of post extubation strider in patients underwent surgical procedure in prone position with general anesthesia.
Our study showed that cut off pressure, CLT for PES and air column width before deflation were insignificantly different between the entire population and PES group. PES occurred only in 15 (20%) patients. When comparing between patients with and without PES, baseline characteristics (age, sex, weight, height, and BMI) had no discernible effect on the examined groups. Disease severity score and intubation period had no discernible effect on the examined groups. Air column width and cut off pressure were inconsequentially different among the researched groups. ACWD was a significant predictor of PES incidence at Cut off value ≤0.8 mm, AUC =0.715, and P=0.02 with 71.43% sensitivity, 78.33 % specificity, 43.5 % PPV, and 92.2 % NPV.
In harmony with our findings, Zytoun et al. [29] found that PES accounted for 20% of the cases, or 20 total cases. In the remaining 75% of cases, PES was not present. Documented ACWD readings were analysed statistically, leading to a recommended cutoff point of <0.9, over which the risk of PES is much increased, with associated values of 80% sensitivity, 90% specificity, 72.7 percent PPV, and 93.1 percent NPV.
Additionally, Ding et al. [26] cases who experienced a stridor had a considerably lower ACWD and ACW during cuff deflation than cases who did not, but no cutoff value was found for predicting PES. Due to the tiny sample size, the results of this research should be taken with caution (n=51), which included just four individuals with PES.
Sensitivity, specificity, and PPV were all identified as low in a current prospective analysis of 41 critically ill cases [17]. US is a potential method to predict effective extubation with respect to laryngeal edema, according to the results of a new prospective observational study involving 101 patients in critical condition [52].
Similar findings were observed in cases who developed PES in research by Sutherasan et al. [17], who also proposed a cutoff value of 1.6 mm for ACWD and showed that ACWD measured with bedside US was highly predictive (sensitivity 70.6%, specificity 70.2%, and NPV 92.2%).
In contrast to our findings, Mikaeili et al. [22] PES was predicted with low sensitivity and specificity using either ACWD or air column width. When comparing CLT and laryngeal US for forecasting PES, CLT still has higher sensitivity and specificity. The limited size of their sample may account for this.
The study was limited by its single-centre design, the fact that bronchoscopy was not possible for all patients, and the inability to standardise ETT sizes across all cases.
Conclusion
The positive predictive value and sensitivity of CLT for predicting PES are minimal. The US measurements of ACWD are an excellent predictor of PES. In addition, larger-scale investigations are necessary to validate our findings. Likewise, additional research, particularly randomised controlled trials, is required to show how helpful this method is in practice as part of the airway examination before extubation. We recommend that airway edema should be reassessed prior to extubation.
Disclosure Statement
No potential conflict of interest was declared by the authors.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors' Contributions
All authors contributed to data analysis, drafting, and revising of the manuscript and agreed to be responsible for all the aspects of this work.
Orcid
Abdel Wahab Abdelsattar Saleh Mohammad
https://orcid.org/0009-0000-5925-6324
Yara Ayman Iskandarani
https://orcid.org/0000-0002-4863-5414
HOW TO CITE THIS ARTICLE
Abdel Wahab Abdelsattar Saleh Mohammad, Yara Ayman Iskandarani, Wael Mohammed Mossa, Maher A sheriff, Mohamrd Hamdi Alqassas. Comparative Study between Cuff Leak Test and Laryngeal U/S for Detection of Post Extubation Oedema in Prone Position Patient with General Anesthesia. J. Med. Chem. Sci., 2023, 6(11) 2686-2698.


