Document Type : Original Article
Authors
- Tarosa Yodia Urolita 1
- Nurwasis . 1
- Ismi Zuhria 1
- Fariztah Sukainah Nur Fathimah 1
- Annisa Karima 2
- Nila Kurniasari 3
- Djoko Agus Purwanto 4
- Eko Budi Koendhori 5
1 Department of Ophthalmology, Faculty of Medicine, Airlangga University, Dr. Soetomo General Academic Hospital, Surabaya, Indonesia
2 Department of Ophthalmology, Faculty of Medicine, Universitas Airlangga/Dr. Soetomo Public Academic Hospital, Surabaya, Indonesia
3 Department of Anatomical Pathology, Faculty of Medicine, Airlangga University, Dr. Soetomo General Academic Hospital, Surabaya, Indonesia
4 Department of Clinical Pharmacy, Faculty of Pharmacy, Airlangga University, Surabaya, Indonesia
5 Department of Microbiology, Faculty of Medicine, Airlangga University, Surabaya, Indonesia
Abstract
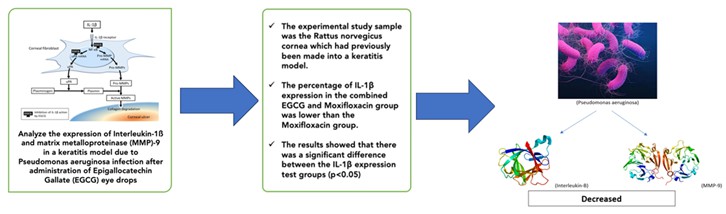
Introduction: Pseudomonas aeruginosa keratitis is the most prevalent eye infection, known to potentially lead to endophthalmitis and corneal perforation. Although antibiotic therapy effectively eliminates the bacteria, the damage induced by toxins in the cornea persists, resulting in corneal thinning, perforation, or fibrosis. The healing process of the corneal wound is influenced by Interleukin-1β and matrix metalloproteinase-9 (MMP-9). Epigallocatechin gallate (EGCG), possessing antibacterial, anti-inflammatory, and antioxidant properties found in Camellia sinensis extract, holds promise as an adjuvant therapy for bacterial keratitis. This study aims to analyze the expression of Interleukin-1β and matrix metalloproteinase-9 (MMP-9) in a keratitis model induced by Pseudomonas aeruginosa infection following the administration of Epigallocatechin Gallate (EGCG) eye drops (an experimental study conducted on Rattus norvegicus rat models).
Methods: The experimental study utilized samples of Rattus norvegicus corneas, previously induced to form keratitis models, with 6 samples each in the negative control group, Moxifloxacin group, and combined Moxifloxacin and EGCG group. Results: The percentage of Interleukin-1β expression in the combined EGCG and Moxifloxacin group was lower compared to the Moxifloxacin group. The results indicated a significant difference in the Interleukin-1β expression among the test groups (p < 0.05). The post hoc test revealed significant differences between the Moxifloxacin group and the combined EGCG group (p < 0.05), as well as between the negative control group and the combined EGCG group (p < 0.05). The mean percentage of MMP-9 expression in the combined EGCG group was lower than that in the Moxifloxacin group. The One-way ANOVA test indicated a significant difference among the three treatment groups (p < 0.05).
Conclusion: There was a significant reduction in the expression of Interleukin-1β and MMP-9 in animal models of keratitis induced by Pseudomonas aeruginosa infection following the administration of Epigallocatechin Gallate (EGCG) eye drops.
Graphical Abstract
Keywords
Introduction
Pseudomonas aeruginosa keratitis is the most prevalent eye infection [1, 2]. It develops rapidly and can lead to ocular infections such as endophthalmitis and corneal perforation, resulting in vision loss [3-5]. Antibiotic therapy efficiently eradicates the bacteria [6-15], but the corneal damage induced by toxins persists [8]. The inflammatory process leads to corneal thinning, corneal fibrosis, and even corneal perforation [16]. The development of scar tissue on the cornea is a chronic complication that may interfere with vision, potentially leading to blindness [17, 18]. The corneal wound healing process is influenced by Interleukin-1β and matrix metalloproteinase (MMP) [19, 20]. Interleukin-1β, a proinflammatory cytokine, is secreted by various immune cells in response to both acute and chronic inflammation. It has a key role in the regulation of the host response to bacterial infection including those associated with corneal ulcer [21]. Conversely, matrix metalloproteinase (MMP) refers to a group of proteolytic enzymes implicated in the pathogenesis of several ocular surface diseases [22-25]. Diseases of the ocular surface are often associated with MMP overexpression so they can provide diagnostic data for ocular surface diseases. B cell-activated nuclear factor kappa light-chain (NF-kB) binds to the MMP-9 DNA promoter site to increase the amount of MMP-9 mRNA. NF-kB inhibition indicates a decrease in MMP-9 transcriptional activity and growth of limbal epithelial cells after inflammation or injury to the ocular surface. These cellular changes affect tissue remodeling, epithelial migration, and vascular proliferation [26, 27].
The primary treatment for Pseudomonal keratitis involves administering appropriate antibiotics to halt the microbial invasion process, alongside NSAIDs or steroids to mitigate the inflammatory response. However, this treatment has not proven effective in inhibiting further destruction resulting from severe inflammatory processes [28, 29]. Tissue regeneration is also suboptimal due to the persistent inflammatory process, even after the causative bacteria have been eradicated [30]. Epigallocatechin Gallate (EGCG), with its antibacterial, anti-inflammatory, and antioxidant properties found in Camellia sinensis extract, holds promise as an alternative adjuvant therapy in the treatment of bacterial keratitis [31]. Recent research suggests that EGCG possesses anti-inflammatory and antioxidant effects on various cell types, including corneal cells [31, 32]. EGCG has been observed to inhibit the activation of pro-MMP-9, a protein generated by corneal fibroblasts in response to Interleukin-1ß stimulation. This inhibitory effect seems to be facilitated by the suppression of uPA upregulation, while pro-MMP-9 expression remains largely unaffected. Existing literature suggests that EGCG has the ability to impede collagen formation or breakdown in numerous cellular populations [33-36].
Sugioka stated that EGCG's inhibitory effect on Interleukin-1ß is concentration-dependent, with significant concentrations observed at 30, 100, and 300 μM [33]. Various studies have examined the effectiveness of Epigallocatechin Gallate (EGCG) as an antimicrobial, anticancer, and antioxidant [37-45]. However, no studies have investigated the effectiveness of EGCG eye drops on the expression of Interleukin-1β and MMP-9 in Pseudomonal keratitis. Based on this background, this study aims to analyze the effectiveness of EGCG eye drops on the expression of Interleukin-1β and MMP-9 in Pseudomonal keratitis. The hypothesis of this study is there were differences in the expression of Interleukin-1β, MMP-9 between the group given moxifloxacin, combination of moxifloxacin and EGCG, and the negative control group in an animal model of keratitis due to Pseudomonas aeruginosa infection.
Materials and Methods
The research employed an experimental design, specifically utilizing a post-test-only control group design. The investigation was conducted at the Faculty of Veterinary Medicine, Airlangga University, Surabaya, Indonesia, from September to October 2022. Rats were chosen as experimental animals because they have advantages for bacterial keratitis, compared to rabbits which are superior in examining conjunctival and anterior chamber abnormalities also there are many commercially available reagents for analyzing mouse-specific factors. Ethical clearance was obtained from the veterinary faculty after an evaluation and trial with 5 consultants until we obtained approval for the research according to the animal ethical code. A total of 18 Wistar adult male white rats (Rattus norvegicus) were included in the study through random allocation. The sample size was determined by replication formula and it takes minimal of 6 rats in every group. The samples were divided into a test group (combined Moxifloxacin 0.5% and EGCG 0.005% group) and a control group, consisting of a negative control group receiving NaCl 0.93% and benzalkonium chloride (BAK) 0.1% solution, and a Moxifloxacin 0.5% group as a positive control. The subjects were Wistar white rats, male, aged 3-4 months, weighing 250-300 g. The health status of the rats was assessed by a veterinarian at the Faculty of Veterinary Medicine, Universitas Airlangga. Rats meeting the inclusion criteria received a corneal epithelial defect using a 1 mm long scratching technique in three places at the center of the right eye's cornea. Subsequently, a 5 µl suspension containing Pseudomonas aeruginosa (106 CFU) was induced. All groups were observed for 48 hours without administering antibiotics or other treatments. Afterward, the surface of the eyeball was examined, and a random allocation was performed into three groups: negative control (K1), Moxifloxacin 0.5% (K2), and combined EGCG (K3) groups. In this study, observations of the eyeball surface were conducted on the first day (prior to the induction of Pseudomonas aeruginosa keratitis), third, and fifth days using a handheld slit lamp. The fluorescence test was performed by applying fluorescein dye to the eye, followed by irrigation with sterile distilled water. The corneal condition was evaluated using a slit lamp (biomicroscope) under blue light. Following induction, the subjects were randomly allocated. The treatment was initiated on the third day, 48 hours after the induction of bacterial keratitis. The K1 group received one drop of combined NaCl 0.93% and benzalkonium chloride (BAK) 0.1% eye drops every 4 hours. The K2 group received one drop of moxifloxacin 0.5% every 4 hours. The K3 group received combined Moxifloxacin 0.5% and EGCG 0.005% eye drops every 4 hours, with a 5-minute interval between drug administrations. On the third and fifth days, observations of the eyeball surface were carried out, including measuring the size of the corneal epithelial defect. Subsequently, all experimental animals were euthanized and enucleated for immunohistochemical examination of Interleukin-1ß and MMP-9 expression. The enucleated rabbit eyes were fixed in a 10% buffered formalin solution to inhibit autolysis and decomposition. The fixation process lasted 24 hours at room temperature. Following fixation, the eyes were embedded in paraffin for further analysis. The corneal tissue, separated from other tissues, was immersed in a 10% neutral buffered formalin (NBF) solution and left to fixate for 48 hours at room temperature. The fixed tissue specimen dimensions were 20 mm x 30 mm, with a thickness ranging from 2 to 4 mm. To ensure successful fixation, a ratio of 2 ml of formalin was used for every 100 mg of tissue. The paraffin block was sectioned into 4 μm thick slices using a microtome. The specimens were placed on polylysine glass objects and incubated at 45 °C overnight. The preparations were paraffinized, washed with distilled water, incubated with 3% H2O2 for 3 minutes, and washed again. Subsequently, the preparations were incubated with pH 6 citrate buffer at 95 °C for 45 minutes, cooled for 30 minutes, and washed with PBS 2x for 3-5 minutes. The preparations were then incubated with blocking serum for 15 minutes, drained, incubated with primary antibodies at a 1:300 dilution for 60 minutes, and washed with PBS 2x for 3-5 minutes. Next, incubation with secondary antibodies was carried out for 20 minutes, followed by washing with PBS 2x for 3-5 minutes. Preparations were incubated with HRV Avidin for 10 minutes, washed with PBS 2x for 3-5 minutes, and DAB chromogen (1:50) was applied for 2 minutes. After washing with running water, counterstaining was performed with Meyer's hematoxylin, followed by washing with running water. The final step involved dipping in graded alcohol (70%, 96%, and 100%), xylol, and mounting. The expression levels of Interleukin-1ß and MMP-9 were observed in representative fields at 400x magnification, displaying a brown color with good intensity. The results were quantified as percentages. Data were recorded and analyzed using the One-way ANOVA test because the data is parametric with 3 groups and because result is significant then followed by a post hoc test to compare 2 groups and shows which groups is significant. Statistical significance was considered if the p-value was < 0.05. SPSS software was utilized for statistical analysis.
Results and Discussion
Clinical scores for corneal inflammation before and after exposure were observed using a handheld slit lamp. The fluorescence test revealed corneal defects in all subjects, which were assessed using clinical scores. All subjects obtained clinical scores of 2 and 3. A clinical score of 2 indicates corneal inflammation resulting in a hazy cornea, partially or completely covering the pupil, while a clinical score of 3 signifies a hazy cornea covering the entire anterior segment (Figures 1 and 2).
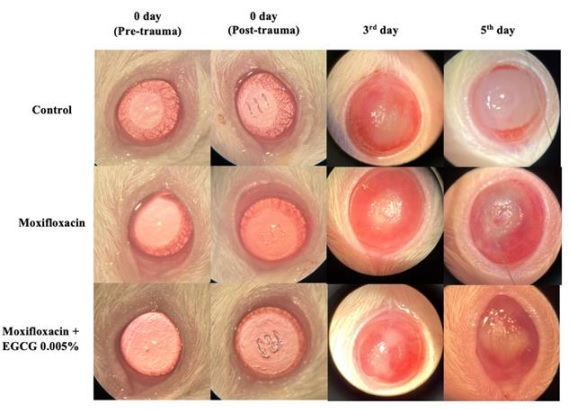
Figure 1: Clinical stages of the three groups (K1, K2, and K3) before and after induction on the 3rd and 5th days after treatment. On the control group shows significant hazier cornea (the whitish appearance) on the 3rd and 5th day. On moxifloxacin group shows hazier and increase in size. On moxifloxacin+EGCG 0.005% the hazy and size persist
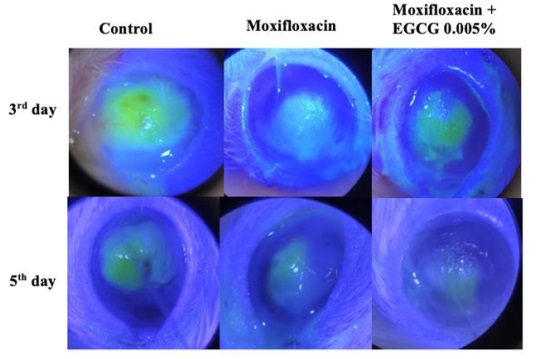
Figure 2: Fluorescein examination of the three groups (K1, K2, and K3) on the 3rd and 5th days. The dye fluoresce under the cobalt blue light shows corneal abrasion. On the moxiflocaxin and moxifloxacin + EGCG 0.005% group shows the dye on the 5th day less than in the 3rd day means the abrasion is healing. On the control group the dye relatively, the same size on the 3rd and the 5th day
In the clinical examination on the 3rd day, the mean clinical scores for K1, K2, and K3 were 2.17 ± 0.41. On the 5th day, the mean clinical scores for K1, K2, and K3 were 2.67 ± 0.52, 2.5 ± 0.55, and 2.33 ± 0.52, respectively (Table 1). This result demonstrates a reduction in the degree of clinical score with each treatment. The slit lamp examination shows clearer cornea on group K2 and K3 on the 5th day compared to the 3rd day.
The results of the Kruskal-Wallis test indicated that there was no statistically significant variation in clinical scores between the K1, K2, and K3 groups on both the third day (p=0.97) and the fifth day (p=0.53). It is important to note that statistical significance is often defined as a p-value less than 0.05. The expression of Interleukin-1β and MMP-9 is quantified as a percentage, calculated based on the area occupied by cells expressing Interleukin-1β and MMP-9, as observed under a light microscope at a magnification of 400x. This analysis is conducted throughout all representative fields of the cornea. The immunohistochemical study using Hematoxylin-eosin staining, along with the application of anti-Interleukin-1β and anti-MMP-9 antibodies, revealed the expression of Interleukin-1β and MMP-9 in the area affected by Pseudomonas aeruginosa keratitis, as observed in the comparison across different groups (Figure 3). The cytoplasm of cells exhibiting Interleukin-1β and MMP-9 expression is characterized by a brown coloration.
Table 1: Mean Clinical score and expression levels of interleukin-1ß and MMP-9
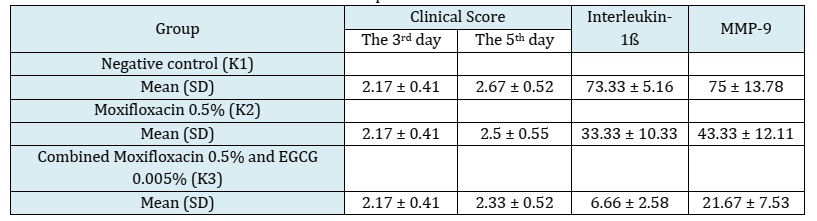
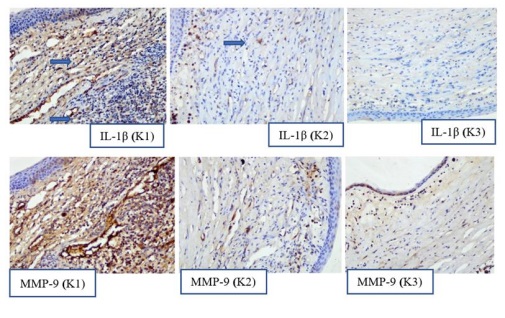
Figure 3: Interleukin-1ß and MMP-9 expression in areas of Corneal Keratitis: K1 Group (Combined NaCl 0.93% and Benzalkonium Chloride (BAK) 0.1% Eye Drops), K2 Group (Moxifloxacin 0.5% Eye Drops), and K3 Group (Combined Moxifloxacin 0.5% and EGCG 0.005% Eye Drops) (Immunohistochemical Staining, 400x Magnification)
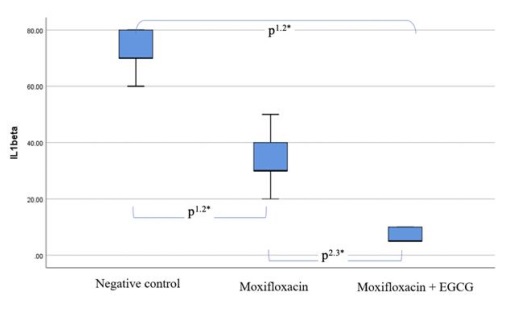
Figure 4: Interleukin-1β expression among the K1 Group (Combined NaCl 0.93% and Benzalkonium Chloride (BAK) 0.1% Eye Drops), K2 Group (Moxifloxacin 0.5%), and the K3 Group (Combined Moxifloxacin 0.5% and EGCG 0.005%) (Significant if p < 0.05; p = 0.000, *), Post hoc test: p1.2, p1.3, and p2.3 = 0.000
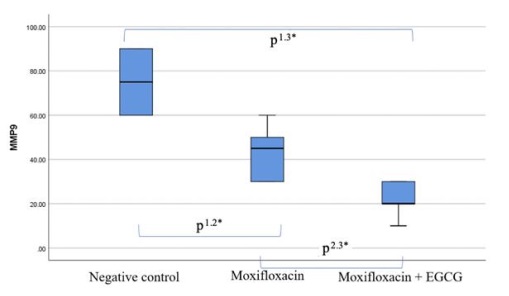
Figure 5: MMP-9 expression among the following groups: K1 Group (Combined NaCl 0.93% and Benzalkonium Chloride (BAK) 0.1% Eye Drops), K2 Group (Moxifloxacin 0.5%), and K3 Group (Combined Moxifloxacin 0.5% and EGCG 0.005% (Significant if p < 0.05; p = 0.000, *), Post Hoc test: p1.2=0.001; p1.3 = 0.000; and p2.3 = 0.015
The mean expression level of Interleukin-1β among K1, K2, and K3 showed a decrease with each treatment. The results indicated that the mean expression level of INTERLEUKIN-1β percentage in the K3 group was lower than in the K2 group (21.67±7.53 vs. 43.33±12.11). The One-way ANOVA test analysis (Figure 4) demonstrated a significant difference among the K1, K2, and K3 groups (p < 0.05). The results of the post hoc test, adjusted for Bonferroni (since the homogeneity of variance test yielded consistent variances, while the Games Howell test would have been used if variances were not homogeneous), indicated a significant difference between the K1 and K2 groups, K1 and K3 groups, as well as the K2 and K3 groups (p < 0.05) (Figure 4). Observations presented in Table 1 revealed that the average percentage of MMP-9 expression in the control group receiving a combination of NaCl and BAK solution was 75 ± 13.78, with a notably large standard deviation, indicating considerable data variation. In the positive control group and the test group, the percentages were 43.33 ± 12.11 and 21.67 ± 7.53, respectively. These results indicate that among the three treatment groups, the negative control group had the highest percentage of MMP-9 expression, while the combined EGCG group had the lowest percentage.
The results demonstrate that MMP-9 expression, an enzyme involved in the inflammation and tissue remodeling process, is lower with Moxifloxacin 0.5% therapy compared to the combined NaCl solution therapy and even lower in the combined EGCG therapy. This highlights the role of EGCG as an adjuvant in the healing and tissue remodeling process. The combined EGCG group exhibited the smallest whisker box size among the treatment groups, indicating that the variation in the combined EGCG group is the smallest among the others. The One-way ANOVA test results (Figure 5) demonstrated a significant difference among the three MMP-9 expression groups shows the differences are meaningful enough to be able to consider the effects of the treatment.
The process of corneal wound healing is characterized by its distinctiveness and complexity. In contrast to other organs, the cornea is characterized by its avascular nature [9]. The cornea is an organ that possesses transparency as a fundamental characteristic. The transparency maintenance in wound healing and the prevention of excessive fibrotic processes are important aspects to consider [46, 60]. The corneal lesion characteristic in Pseudomonas keratitis is a corneal ulcer with a ring-shaped abscess. These lesions develop rapidly and often result in corneal perforation, leading to blindness [10-14]. Following the occurrence of a corneal epithelial defect, there is a migration and proliferation of cells to cover the damage. The death of epithelial cells triggers the release of Interleukin-1 into keratocytes, which subsequently undergo apoptosis due to Interleukin-1 exposure. The extent of corneal damage correlates with the extent of apoptotic keratocytes [47]. This process of keratocyte apoptosis serves as a defense mechanism to limit the spread of foreign substances, such as microbes, into deeper tissues. Keratocytes that do not undergo programmed cell death, known as apoptosis, can be induced to differentiate into fibroblasts, depending on the degree of interleukin-1 exposure. Fibroblasts play a critical role in initiating cellular differentiation, migration, and proliferation processes that contribute to wound closure [27]. In P. aeruginosa keratitis, the development of corneal ulcers occurs rapidly, primarily due to the production of elastase and alkaline protease by P. aeruginosa, which can degrade corneal collagen. Collagen and corneal structures are damaged as a result of proteases produced by bacteria and the activation of corneal fibroblasts [34]. P. aeruginosa also produces exotoxins, such as exotoxin-A, phospholipase, and hemolysin, which can alter the corneal structure and activate endogenous corneal proteases. In addition, these bacteria can suppress the host immune response by interfering with key proteins and mediators, including IgA, IgG, interleukins, complement, and gamma interferon (IFN-γ) [48]. The clinical score results align with the idea that antibiotics can eliminate bacteria, reducing the cause of collagen degradation from bacteria. However, the degradation of corneal collagen will continue due to the activation of the corneal fibroblasts, even though the bacterial factor has been eliminated [35]. The intense inflammatory process results in less effective antibiotic therapy due to the toxin produced by P. aeruginosa. While antibiotic therapy can rapidly eliminate bacteria, it does not halt corneal damage [17, 18]. Epigallocatechin gallate (EGCG), found in Camellia sinensis extract, holds promise as an anti-inflammatory and antioxidant for use as an adjuvant therapy in bacterial keratitis. Recent studies suggest that EGCG has anti-inflammatory and antioxidant effects on various cell types, including those in the cornea [31].
Effectiveness of EGCG on interleukin-1β expression in P. aeruginosa keratitis
The observed reduction in INTERLEUKIN-1β expression in the combined EGCG therapy (K3 group) compared to the Moxifloxacin group aligns with findings from previous studies [33, 48-53]. Akhtar and Haqqi (2011) concluded that EGCG can inhibit the expression of 29 proteins regulated by INTERLEUKIN-1β in human chondrocytes. The study also reported EGCG's ability to inhibit various inflammatory mediators, including epithelial neutrophil-activating peptide-78 (ENA-78), granulocyte-macrophage colony-stimulating factor (GM-CSF), growth-related oncogenes (GRO), GRO-α, interleukin-6 (IL-6), interleukin-8 (IL-8), monocyte chemotactic protein-1 (MCP-1), MCP-3, macrophage inflammatory protein-1beta (MIP-1β), granulocyte chemotactic protein-2 (GCP-2), MIP-3alpha, interferon-gamma-inducible protein-10 (IP-10), nucleosome assembly protein-2 (NAP-2), and leukemia inhibiting factor (LIF). The primary mechanism via which EGCG exerts its inhibitory action is by suppressing the activation of NF-κB and c-Jun N-terminal Kinase (JNK)-MAPK [49]. These findings are consistent with Sugioka et al. (2019), who stated that EGCG inhibits INTERLEUKIN-1β-induced degradation of plasminogen-dependent collagen by corneal fibroblasts, with the effect varying with concentration. It was observed that EGCG attenuates INTERLEUKIN-1β-induced expression of uPA at the mRNA and protein levels [50]. EGCG also inhibits INTERLEUKIN-1β-induced conversion of exogenous plasminogen to plasmin, as well as pro-MMP1-dependent activation of plasminogen [33]. In addition to its anti-inflammatory and antioxidant effects, EGCG also exhibits antibacterial properties, as stated by Zhao et al. (2013). EGCG can interact with various proteins and exert multiple antibacterial activities by disrupting microbial cytoplasmic lipids and proteins [36, 51]. Stapleton et al. (2004) reported that EGCG, at specific doses, provides protection against severe polymicrobial infections and significantly reduces bacterial counts, particularly in the liver and lungs [52]. Sudano et al. (2004) suggested that EGCG's mechanism of action involves damaging the activity of the cytoplasmic membrane pump, leading to an increase in the intracellular concentration of antibiotics, suggesting the potential of EGCG as a reliable adjuvant in antibacterial therapy [53]. Furthermore, Chandra et al. (2012) noted that EGCG can interact with various proteins, inducing changes in protein conformation and highlighting its role as a potent protein remodeling agent [54].
Effectiveness of EGCG in regulating interleukin-1β expression in P. aeruginosa keratitis
The results of MMP-9 expression in this study align with Wilson (2021) and Bowie and O'Neill (2000), who emphasized that Interleukin-1β plays a role in increasing pro-MMP-9 levels in the culture medium depending on a specific dose (0-20 ng/ml). Interleukin-1ß can stimulate the promoter activity of the MMP-9 gene, as evidenced by the Moxifloxacin group and the combined EGCG groups expressing lower INTERLEUKIN-1β and MMP-9 compared to the combined NaCl group, serving as the negative control [20, 26]. Jamerson et al. (2020) reported that neutralizing MMP-9 in infected mice resulted in a reduced number of Langerhans cells, a decrease in the number of PMNs, and a reduction in clinical disease severity. These results are consistent with Sugioka et al. (2019), who noted that EGCG inhibited Interleukin-1ß-induced degradation of plasminogen-dependent collagen by corneal fibroblasts, an effect influenced by concentration. This inhibitory action attenuated Interleukin-1ß-induced expression of uPA at both mRNA and protein levels. EGCG also hindered Interleukin-1ß-induced conversion of exogenous plasminogen to plasmin, as well as pro-MMP1-dependent activation of plasminogen in a 3D culture without exerting a substantial effect on excessive pro-MMP1 [33, 55]. EGCG further downregulated MMP 3, MMP 8, and MMP 9 in gingival macrophage and fibroblast cultures [23, 35]. In this study, significantly lower MMP-9 expression was observed in the combined EGCG group compared to the Moxifloxacin Group, corroborating Tanabe et al.'s (2023) conclusion that EGCG holds potential as an anti-MMP agent [56]. Multiple studies examining EGCG's effects as an antimicrobial, anti-inflammatory, antioxidant, and anti-cancer agent have also obtained results consistent with our findings [57-61].
Conclusion
Epigallocatechin Gallate (EGCG) demonstrated a significant reduction in Interleukin-1ß and MMP-9 expression levels in the combined EGCG and Moxifloxacin group compared to the Moxifloxacin group in animal models of Pseudomonas aeruginosa keratitis [61]. The findings of this study shows that the EGCG could become the adjuvant therapy for Pseudomonas aeruginosa keratitis proved by the combined moxifloxacin and EGCG group were superior than other groups. However, this research has several limitations. Clinical scores were only observed on the third and fifth day after therapy, and longer observations are needed to understand the complete healing process of the corneal wound. Further studies to observe serial expression of Interleukin-1β and MMP-9 until the wound healing process is complete is needed because the cytokine expression occurs dynamically based on the state of the wound healing process while this study was conducted only once. Serial observation of the Interleukin-1β and MMP-9 expression percentages is necessary.
Acknowledgments
We would like to express our gratitude to the Faculty of Veterinary Medicine, Universitas Airlangga, for providing the necessary assistance, materials, and facilities for this research. Our sincere appreciation goes to Dr. Arief Wibowo, MS. (Faculty of Public Health, Universitas Airlangga), for his valuable statistical and methodological advice, and to Drh. Djoko Legowo (Faculty of Veterinary Medicine, Universitas Airlangga) for granting ethical clearance.
Conflict of Interest
The authors declare no conflicts of interest in relation to this study.
Funding
This study was supported by the Ministry of Research, Technology, and Higher Education, Indonesia.
Authors’ Contribution
All authors contributed equally to this study and the publication of this manuscript.
ORCID
Tarosa Yodia Urolita
https://orcid.org/0009-0009-7297-0536
Nurwasis
https://orcid.org/0000-0001-8302-729X
Ismi Zuhria
https://orcid.org/0000-0003-2102-7782
Fariztah Sukainah Nur Fathimah
https://orcid.org/0009-0004-1539-1945
Annisa Karima
https://orcid.org/0009-0004-0183-4362
Nila Kurniasari
https://orcid.org/0000-0001-5584-2705
Djoko Agus Purwanto
https://orcid.org/0000-0002-2718-903X
Eko Budi Koendhori
https://orcid.org/0000-0002-4412-0755
HOW TO CITE THIS ARTICLE
Tarosa Yodia Urolita, Nurwasis*, Ismi Zuhria, Fariztah Sukainah Nur Fathimah, Annisa Karima, Nila Kurniasari, Djoko Agus Purwanto, Eko Budi Koendhori, The Effectiveness of Epigallocatechin Gallate (EGCG) Eye Drops to Interleukin -1ß and Matrix Metalloproteinase (MMP)-9 Expression in Pseudomonas Aeruginosa Keratitis: An In Vitro Approach. J. Med. Chem. Sci., 2024, 7(3) 461-473.