Document Type : Review Article
Authors
1 Assistant Professor of Emergency Medicine, Department of Emergency Medicine, School of Medicine, Shahid Sadoughi University of Medical Sciences, Iran
2 Department of Cellular and Molecular Biology, Faculty of Basic Sciences, Rafsanjan University, Iran
3 BSc in Anesthesiology at Shahrekord Medical University, Iran
4 Researcher at the Anesthesia and Pain & Molecular and cell Biology Research center, Faculty of Medicine Department of Anatomy, Iran university of Medical Sciences, Tehran, Iran
5 Department of Emergency Medicine, Khatam-Al-Anbia Hospital, Zahedan University of Medical Sciences, Zahedan, Iran
6 Clinical Immunology Research Center at Zahedan University of Medical Sciences, Zahedan, Iran
Abstract
This study is a conceptual review. Various protocols have been proposed for non-communicable diseases worldwide. The importance of this large group of diseases has prompted the World Health Organization (WHO) to plan effectively to set targets to reduce mortality from these diseases by one-third by 2030 in the Sustainable Development Plan. In asthma, corticosteroids are still recognized as the most potent anti-asthma drugs, and there is still no drug with the same effect, and biological agents (drugs such as amalizumab) significantly improve the management of severe asthma. Regarding diabetes, the recommendations of the WHO were reviewed, and the first recommendation is that if metformin, which is recommended as the first oral antidiabetic drug in all guidelines, cannot control hyperglycemia, sulfonylurea should be prescribed to patients with type 2 diabetes. Non-communicable diseases in Iran cause 45% of the disease burden in men and 33% of the disease burden in women, of the total causes of the disease burden in both sexes (6-10). Obesity and overweight, arterial hypertension, inadequate physical activity and addiction are 86% of the risk factors for diseases and 11% of all diseases. These risk factors have caused 6.1 million years of adapted life expectancy in Iran.
Graphical Abstract
Keywords
Main Subjects
Introduction
Given the increasing prevalence of non-communicable diseases in the world, in order to properly implement the care system for non-communicable diseases risk factors and to access reliable and comparable information of these major risk factors, WHO has devised step-by-step approach (STEPs) care for risk factors for these diseases. Accordingly, this inquiry was implemented in this direction [1-3]. The WHO’s step-by-step approach to caring for risk factors for non-communicable diseases has three levels of data collection [4-6]:
Step 1: Questionnaire: smoking, and diabetes and other things such as using the front passenger seat belt and health insurance coverage [7];
Step 2: Laboratory tests: including fasting blood sugar and blood lipids [8]; and
Step 3: Respiratory tract disease progresses gradually and in the long run leads to a decrease in physical, mental, social and economic ability [9].
Respiratory diseases are on the rise around the world and affect the health and quality of life of millions of people each year. Chronic respiratory diseases and acute respiratory infections are responsible for many hospitalizations and deaths and require complex treatments. In these diseases, it is difficult to transfer drugs to a specific target site with a controlled release rate [10]. To control and prevent the progression of obstructive pulmonary disease, pharmacological and non-pharmacological treatment is performed and in case of failure, the rescue of the patient with lung transplantation is possible [11]. In a study on the evaluation of drug use patterns for patients with asthma, it was shown that physicians should be aware of recent guidelines in the management of asthma and provide the correct drug treatment [12]. Therefore, timely and correct medical treatment is of great importance. Another non-communicable disease is diabetes. Today, diabetes is one of the global challenges and the prevalence of this disease in the world is estimated by 1 to 2 percent and in Iran 3 to 5 percent, which annually adds 100 thousand new cases to patients. About 90% of these patients have type 2 diabetes. Diabetes is the fourth leading cause of death in developed countries [13]. The chronic nature of diabetes affects the patient's body, mind and individual and social functioning [14]. Pharmacological treatment is one of the inevitable ways to treat diabetic patients. There are various protocols for treating diabetes [15-17].
Given that dysfunctional and poor control of non-communicable diseases increases costs and harm to patients, the goal of treatment is primarily to preserve life and reduce the symptoms of the disease. The second goal is to prevent long-term side effects by eliminating a variety of risk factors to increase life expectancy, so effective treatment of these patients using new and approved therapeutic drugs, is very important in reducing costs. Therefore, this study was conducted to evaluate drug therapy in non-communicable diseases in the form of a review study and the most widely used drugs that are potentially used to treat non-communicable diseases are briefly reviewed [18-20]. Increasing cases of non-communicable diseases around the world have made the disease a public health priority in the poorest countries, according to Wifrom. Many chronic diseases, such as cardiovascular diseases, diabetes, chronic respiratory diseases, including asthma, and some cancers, can be controlled with medication and can prolong life through strong primary health systems. However, many people with non-communicable diseases in low-income countries strive for early, effective diagnosis and access to the medicines they need. More cost and less access are an important issue here. Surveys in more than 40 countries have shown that access to public medicines for the treatment of chronic diseases in the public and private sectors is generally more difficult than for medicines for acute diseases. The price of these drugs is much higher than the real prices in many countries, so patients face problems, and if governments can provide quality drugs at affordable prices, it will obviously make it possible to expand services and treatment to a wider segment of the population. Consolidated procurement strategy seeks to consolidate market demand and increase demand transparency. This can give manufacturers easy access to the market and give buyers more bargaining power to ensure quality and guarantee supply at a reasonable price. In essence, integrated purchasing can reduce transaction costs, consolidate fragmented markets, and enable more accurate collection of market information. Some integrated procurement schemes have improved access to medicines for diseases such as HIV, AIDS and malaria, especially in low- and middle-income countries. For example, the procurement mechanism collected by the World Fund in 2019 alone managed about $ 1 billion in orders and services to 63 countries and $ 174 million in treatment and diagnosis costs for diseases such as AIDS and malaria, but improved access to NCD drugs is not easy, and many more drugs are needed for non-communicable diseases (excluding cancer) and more manufacturers. Global and regional competition can lower prices and increase efficiency, but when you look at the number of registered manufacturers in countries, the market structure changes. For some drugs, many manufacturers are registered and for some, few manufacturers are registered. Finally, the market is failing for a variety of reasons (related to local demand and capacity and purchasing policies) and different solutions are needed that vary from country to country. The mass procurement of NCD drugs is also hampered by a lack of resources [21-23].
Material and Methods
This study is a conceptual review relying on searching and extracting research-related studies. First, researchers searched for the relevant articles. Researchers first extracted related keywords using the MeSH strategy.
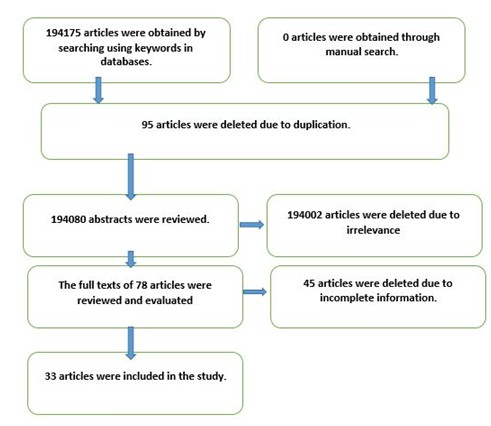
Figure 1: The shematic of Method
Search for resources using the keywords non-communicable diseases, diabetes, hypertension, asthma, chronic respiratory diseases, drug treatment, medicine in Persian databases Barekat, Iran Medex, Irandoc, Magiran, SID and using the keywords English Non-communicable diseases, Diabetes, Hypertension, Asthma, Chronic respiratory diseases, Pharmacotherapy, Medication, Treatment were performed in Google Scholar, Scopus, science direct, PubMed, web of science databases from 2013 to 2021 in September and October 1400. The words were searched separately as well as in combination of two words using Boolean operators. In order to increase the validity of the study findings and control the bias in data entry, the search process, selection of studies and decision-making on entering or constructing the study and evaluation of the full text of the articles were performed by two independent browsers. This process was evaluated by a third party [24-26].
Extracting articles according to inclusion criteria
Using the above keywords at the end of the search, including 60150 articles from Persian databases and 134025 articles from international databases and a total of 194175 studies were collected. The studies were reviewed based on inclusion criteria. The selection of related studies was done in such a way that first a list of titles and abstracts of all articles in databases was prepared by researchers. And if after reading the title and abstract, it was not possible to make a decision about the study, the full text was studied. Then, the related articles were independently entered into the research process and finally 33 articles were included in the study.
Tabulation and summarization of information and data
At this stage, after the data were extracted, all study data were summarized based on the name of the first author, year, place, title, tools or research papers in the relevant table.
Reporting the results
After reading the summary and full text of the articles related to the research topic, the required data were extracted for writing, including author name, year, place, type of study, sampling method, data collection tool and results. Finally, the data obtained from the articles were categorized and finally reported in the full text of a review article [27].
Asthma
Different drugs are used in the treatment of asthma, the most important of which are as follows, according to studies [28].
Corticosteroids
Corticosteroids are also known as glucocorticoids in some sources. Corticosteroids are still the most potent anti-asthma drug, and there is still no drug with a similar effect [29]. Patients with asthma should be noted that side effects such as short stature in children, osteoporosis, and metabolic disorders are major barriers to long-term use of these drugs, so scientists have begun to consider the inhaled form of these drugs. So that the drug would act only locally and not cause severe systemic effects [3]. In general, these drugs reduce the expression of genes associated with inflammatory responses and thus suppress and reduce inflammatory responses; however, the presence of these drugs in the treatment of some other respiratory diseases shows less metabolic disturbance [31].
Beta receptor Agonist
Beta-receptor agonists are generally divided into short-acting (SABA) and long-acting (LABA). Inhaled short-acting drugs such as salbutamol and turbotalin are the most effective bronchodilators available for the rapid recovery of asthma. Formotrol is also known as a long-acting drug.
Salbutamol is the most widely used anti-asthmatic drug, which activates protein kinase A by activating an intracellular messenger. This protein then steps down the myosin kinase enzyme to phosphorus, relaxing the smooth muscles of the bronchi. As a result, the bronchial obstruction caused by asthma is relieved.
Long-acting drugs, including formotrol and salmeterol, induce bronchodilation for at least 12 hours and are used as adjunctive therapy for uncontrolled asthma with corticosteroid inhalers.
It should be noted that single-drug treatment with these drugs is not recommended because they obscure the intensifying inflammatory effects [32].
Muscarinic receptor antagonists
Both atropine and scopolamine are of plant origin. These two drugs are muscarinic receptor athenogens. Atropine and scopolamine were used as relatively effective bronchodilators before the introduction of new bronchodilators, but after the introduction of new drugs, the use of atropine decreased. Ipratropium is a newer drug from the same group of drugs that has a long-acting effect and its bronchodilator effect lasts for several days. Tiotropium is more likely to bind to the M3 receptor. The M3 receptor dilates the bronchi, while the other muscarinic receptor, M2, has an inhibitory effect on parasympathetic nerves. Therefore, tiotropium has fewer side effects than atropine and scopolamine, which are nonspecific antagonists of muscarinic receptors [33].
Mediator antagonists (leukotriene receptor antagonists)
Histamine inhibitors and leukotriene inhibitors fall into two categories. Numerous studies have shown an association between histamine secretion and increased bronchoconstriction and constriction. However, early H1-receptor blocking drugs (such as Mapir Amin) were not very effective in preventing asthma complications, possibly due to the presence and production of bronchoconstrictors other than histamine in the asthma process. Another substance was then identified that, along with histamine, was released during the anaphylactic reaction, causing bronchial obstruction or contraction. These lipid mediators were later named leukotrienes [34].
Inhibitory drugs are leukotriene receptors that, along with histamine, are released during the anaphylactic reaction and cause bronchial blockage or contraction. These include saffron Locast, Montlucast, and Pranlocast, and a cyclooxygenase inhibitor called Zilton. These drugs were introduced for clinical use during the 1990s and have become the only new class of antihistamines in the last 30 years. However, they are less effective than inhaled corticosteroids, but on the other hand, they have benefits such as oral use and fewer side effects.
Phosphodiesterase inhibitors (PDE-I)
Theophylline is a weak non-selective inhibitor of PDEs that is considered a xanthine. Aminophylline is a solution of theophylline that can be administered intravenously. It is very effective in treating severe acute asthma that does not respond to adrenaline. For this reason, before the introduction of Bana 2 agonists, aminophylline became a standard in the treatment of acute cases of asthma. Side effects of these drugs include nausea, vomiting, frequent urination, cardiac arrhythmias, and seizures. Today, with the introduction of beta 2 agonists, theophylline and aminophylline are used only in cases of severe asthma [35].
Immune system modulators
Some older drugs, such as silkosporin A, fall into this category. These drugs stop the function of T cells. Pamycin (Cyrolimus) is another drug that acts by inhibiting calcinurin and has the advantage that it is not nephrotoxic but causes hyperlipidemia (hyperlipidemia) [36].
Allergy immunotherapy (immunotherapy)
This treatment is based on the injection or exposure of the patient or the allergen; allergens are usually given to the person being treated with one of two subcutaneous or subcutaneous methods [37].
Magnesium Sulphate
According to studies, biological agents (drugs such as mopolizumab, amalizumab, dopilumab) significantly improve the management of severe asthma. However, many patients are not treated well. Therefore, there is a need to identify more potential molecular targets and more effective prognosis and biotherapeutic markers, along with a deeper knowledge of cellular and molecular mechanisms, to treat severe or uncontrolled asthma [38]. It has been found that major causes of asthma attacks include exposure to allergens and the use of alcohol and smoking. Reducing smoking helps reduce asthma attacks. Tobacco smoke adheres to patients' moist airways and causes eyelash damage. The most common anti-asthma drugs are beta-2 agonists and corticosteroids, followed by antihistamines and methylxanthines, and a combination of salbutamol with ipratropium bromide and salbutamol with beclomethasone.
Diabetes
The World Health Organization (WHO) has the following recommendations regarding medication for diabetes. The first recommendation is that if metformin, which is recommended as the first oral anti-diabetic drug in all guidelines, fails to control hyperglycemia, sulfonylurea should be prescribed to patients with type 2 diabetes. Although this recommendation does not conform to some guidelines in developed countries, the very low cost of these drugs and their higher potency in reducing HbA1c compared with newer drugs should be taken into account. Obviously, the drug should be avoided in elderly patients as well as those for whom hyperglycemia is dangerous. The second recommendation is to use a simple human insulin injection if the patient with type 2 diabetes is not controlled with metformin plus sulfanilurea. This recommendation is not based on strong clinical evidence; however, the low cost of the drug, its availability, and its high potency in lowering blood sugar have been noted. Studies have shown that when the combination of metformin and sulfanyl urea does not work, only insulin and thiazolidines (compared to placebo) cause a significant reduction in HbA1c. This effect is negligible for DPP-4 inhibitors as well as SGLT-2 inhibitors, although these drugs cause weight loss compared with thiazolidines [39].
The third recommendation is to stop DPP-4 or SGLT-2 inhibitors, as well as thiazolidines, when insulin use is not possible in patients taking metformin and sulfanyl urea; for example, when the patient lives alone and cannot take insulin. Obviously, the power of thiazolidines in lowering blood sugar and HbA1c is preferable to the other two drugs, but it causes weight gain.
The fourth recommendation is to use plain insulin and NPH insulin in patients with type 1 diabetes and type 2 diabetes, which are indicated for insulin use. Because, in terms of diabetes control, there is no difference between this type of insulin and recombinant (analog) insulin products. However, some studies suggest that hypoglycemia with analog insulin may be less likely [40].
Obviously, if plain insulin and NPH are available by pen injection, they can have the advantage of other analog insulins, which make their pen products easier to use. The fifth recommendation is to use long-acting analogues of insulin (glagine and detmir) when diabetics have frequent severe hypoglycemia while taking plain insulin and NPH. It is clear that this recommendation is a definite indication for the use of long-acting analogues and can improve the care of these patients [1].
Blood pressure
Treatment of high blood pressure is very important. According to studies, antihypertensive therapy with a variety of drugs reduces the risk of HF in middle-aged and elderly people, but good adherence to prescribed treatment regimens is an important factor in a significant reduction. This emphasis increases the need for diagnosis by physicians and health care providers and the importance of adhering to the prescribed treatment regimen. Here are some different types of blood pressure medications: You are lying to her [7].
They are a heterogeneous drug group and their pharmacodynamic properties depend on cardiac selectivity, agonist activity, and vasodilation. They all lower blood pressure to the same extent, although the use of different amounts reduces cardiac output and dilates blood vessels attention to their medicinal properties causes.
Diuretics
Thiazide diuretics and ring diuretics increase diuresis. Both can be considered as a major therapeutic class in antihypertensive drugs, although they have two distinct functions. Potassium-preserving diuretics represent another class of therapy [40].
Henle loop diuretics
Furosemide and butanide are in this category.
The mechanism of action
Ring diuretics exert their effect on nephrons in the epithelial membrane of the thick ascending limb of the Henle arc. They reabsorb Na + and chloride in competition with Cl− they inhibit and this leads to increased urinary secretion. These diuretics do not reduce peripheral vasodilation as much as thiazide diuretics. Therefore, they are not comprehensive and are not effective enough in lowering blood pressure [3]. Diuresis rapidly initiates with furosemide, occurs within 1 hour, and peaks in 3-6 hours [2].
Thiazides
Hydrochlorothiazide, chlorthalidone and indapamide are the most widely used thiazide diuretics.
Potassium storage diuretics
This subclass includes competitive aldosterone antagonists, such as spironolactone, apleronone, and drugs that affect aldosterone independently, such as amiloride and triamterene.
Angiotensin converting enzyme inhibitors
Captopril was the first ACEI available for the treatment of hypertension in the early 1980s, followed by analapril, perindopril, lisinopril, ramipril, quinapril, benazepril, silazapril, trendolapril, fusinopril, moxipril, and imidapril.
The mechanism of action
Angiotensinogen protein is converted to angiotensin I by renin, and angiotensin I is converted to angiotensin II by the enzyme converting angiotensin (ACE) in the lungs. Angiotensin II is a potent cause of vasoconstriction (especially of the arteries) and applies a variety of strategies (such as stimulating the secretion of aldosterone and antihypertensive hormone) that cause water and sodium retention, so the ultimate function of angiotensin II is to increase blood pressure. It plays an important role in the treatment of high blood pressure [12].
According to studies, captopril is a safe, uncomplicated, effective, inexpensive, available, and well-known drug for the treatment of hypertension. One study also found that a clinically directed antihypertensive therapy was effective in reversing the inflammatory status of serum cytokines in postmenopausal women and that diuretics and renin-angiotensin system antagonists were highly effective [16].
Angiotensin II receptor blockers
Losartan was the first ARB angiotensin 2 receptor blocker to treat hypertension in the late 1990s, followed by Kandsartan, Aprosartan, Airbusartan, Valsartan, Thelemis Artan and Olmsartan.
The mechanism of action
These drugs are AT1 receptor antagonists and, by inhibiting angiotensin II receptor activation, directly dilate blood vessels, reduce vasopressin production, and reduce aldosterone production and secretion. The result is a reduction in blood pressure [25].
Calcium channel blockers
Calcium channel blockers (CCBs) include verapamil, diltiazem, nifedipine, and amlodipine. They inhibit the entry of calcium into the cell and the exit of calcium from cellular stores. These drugs reduce the rate of atrial-ventricular and sinus-atrial conduction and relax the heart wall muscles and vascular smooth muscle. Binding of calcium to myosin is essential for the contraction of smooth muscle in the arterial wall [11].
Side effects
The ACC / AHA Blood Pressure Guide provides a comprehensive and accurate approach to the diagnosis and treatment of hypertension in adults, despite its differences from other guidelines in the ESC / ESH Guidelines (Figures 2 and 3). Clinical groups have access to almost all published data about everyone. Therefore, the recommendations presented play a key role. The following are guidelines for managing blood pressure treatment (Figure 4).
Until a few years ago, infectious diseases were considered as the biggest health problem in the world, so that all the health resources of the countries were spent on controlling and preventing the spread of these diseases. With the success of the health system and the new technology for several decades, major advances have been made in the control of infectious diseases, and after these steps, non-communicable patients are now a major health problem. The most important diseases in this group include cardiovascular, renal, neurological and psychological diseases, goiter, thalassemia, hypertension, chronic and nonspecific respiratory diseases (such as asthma), permanent consequences of accidents, blindness, diabetes and metabolic, chronic osteoarthritis and cancers.
As mentioned, the reason for this situation is the changes that have been made in people's lifestyles in recent years, and perhaps one of the reasons for these changes, in addition to the requirements of current life, is in people's awareness and behavior. In many cases, lack of sufficient knowledge of risk factors and failure to take the necessary measures, has caused these factors to increase day by day. Therefore, recognizing these factors and policy-making on how to deal with them and reduce their increasing trend can have a significant impact on reducing non-communicable diseases. Chronic and non-communicable diseases seem to be more important among adults in both developed and developing countries. Cardiovascular diseases and cancers are now the leading causes of death in developed countries (Europe and North America), accounting for 70 to 75% of all deaths. In many countries, chronic diseases are on the rise and will increase for a number of reasons. In terms of the incidence of chronic diseases, it is increasing. Another reason is that people's lifestyles and behaviors change rapidly, and this transformation contributes to the onset of chronic diseases. The third reason is that with modern medical care, many people with chronic diseases can survive [35-37].
The impact of chronic disease on people's lives is more serious when it is considered in terms of life expectancy, disability, family difficulties, poverty and the loss of the country's economy. Developing countries have now realized that they need to take steps to avoid the "epidemic" of non-communicable diseases likely to occur along with economic and health development [38-40].

Figure 2: ESC2018 Anti-Hypertensive Drug Treatment Guide [95]

Figure 3: NICE 2019 Anti-Hypertensive Drug Treatment Guide

Figure 4: ISH 2020 Anti-Hypertensive Drug Treatment Guide
Conclusion
The aim of the present study was to evaluate drug therapy in non-communicable diseases. Studies in this area have shown that corticosteroids are still the most potent anti-asthma drug, and there is still no drug with the same effect. Current inhaled and topical corticosteroids, such as fluticasone and budesonide, are modified corticosteroids that are more anti-inflammatory and less metabolic. Salbutamol is the most widely used anti-asthma drug. The effect of leukotriene receptor blocking drugs is less than that of inhaled corticosteroids, but on the other hand they have benefits such as oral use and fewer side effects. According to studies, biological agents (drugs such as mopolizumab, amalizumab, dopilumab) significantly improve the management of severe asthma. Omalizumab should be mentioned as a universal drug for asthma.
Metformin has been used for over 60 years and is still the first drug of choice for T2D. Metformin is used to reduce recurrence in patients with gastric cancer. Metformin is recommended for the treatment of moderate hyperglycemia in pregnancy. The first recommendation is that if metformin, which is recommended as the first oral anti-diabetic drug in all guidelines, fails to control hyperglycemia, sulfonylurea should be prescribed to patients with type 2 diabetes. Adding acarbose to the diet of diabetic patients further reduces the mean fasting blood sugar and blood sugar of patients two hours after eating. Gli Banglamide is a simple, safe, inexpensive and attractive alternative to insulin for the treatment of gestational diabetes. Drug interactions with warfarin or NSAIDs should be carefully monitored to avoid drug side effects.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors' contributions
All authors contributed toward data analysis, drafting and revising the paper and agreed to be responsible for all the aspects of this work.
Conflict of Interest
The authors declare that they have no competing interests.
ORCID
Hamid Mirjalili:
https://www.orcid.org/0000-0002-1268-0395
Maryam Milani Fard:
https://www.orcid.org/0000-0002-0888-8847
Abdolrazaghnejad, Ali:
https://www.orcid.org/0000-0002-4121-1643
HOW TO CITE THIS ARTICLE
Hamid Mirjalili, Hadis Amani, Afsaneh Ismaili, Maryam Milani Fard, Ali Abdolrazaghnejad. Evaluation of Drug Therapy in Non-Communicable Diseases; a Review Study, J. Med. Chem. Sci., 2022, 5(2) 204-214
DOI: 10.26655/JMCHEMSCI.2022.2.8
- Kiarsipour N., Borhani F., Esmaeili R., Zayeri F., Trop. Med. Public Health, 2017, 10:861 [Google Scholar], [Publisher]
- Givi F., Esmaeili R., Mojab F., Nasiri M., Shadnoush M., Koomesh, 2019, 21:254 [Google Scholar], [Publisher]
- Estebsari F., Dastoorpoor M., Khalifehkandi Z.R., Esmaeili R., Aghababaeian H., Aging Sci., 2020, 13:4 [Crossref], [Google Scholar], [Publisher]
- Mohammadi M., Esmaeili R., Fani M., Adv. Pharm. Educ. Res., 2019, 9:111 [Google Scholar], [Publisher]
- Sardari M., Esmaeili R., Ravesh N.N., Nasiri M., Adv. Pharm. Educ. Res., 2019, 9:145 [Google Scholar], [Publisher]
- Hajalimohammadi M., Esmaeili R., Zandi M., Zadeh B.P., Medico-Legal Update, 2020, 20:262 [Crossref], [Google Scholar], [Publisher]
- Azadmehr F., Esmaeili R., Farahani Z.B., Arabborzu Z., Adv. Pharm. Educ. Res., 2018, 8:1 [Google Scholar], [Publisher]
- Esmaeili R., Barziabadi Z.F., Khoob M.K., Nephro-Urol. Mon., 2021, 13:e100728 [Crossref], [Google Scholar], [Publisher]
- Soleimani F., Anbohi S.Z., Esmaeili R., Pourhoseingholi M.A., Borhani F., Clin. Diagn. Res., 12:LC01 [Crossref], [Google Scholar], [Publisher]
- Maddah Z., Ghalenoee M., Mohtashami J., Esmaieli R., Naseri-Salahsh V., J. Islam. Repub. Iran, 2018, 32:1 [Crossref], [Google Scholar], [Publisher]
- Mokhtare M., Alimoradzadeh R., Agah S., Mirmiranpour H., Khodabandehloo N., Middle East J. Dig. Dis., 2017, 9:228 [Google Scholar], [Publisher]
- Etemadi S., Mahmoodiyeh B., Rajabi S., Kamali A., Milanifard M., Romanian Soc. Cell Biol., 2021, 25:2417 [Google Scholar], [Publisher]
- Fard A.M.M., Fard M.M., Eurasian J. Sci. Tech., 2021, 1:284 [Crossref], [Google Scholar], [Publisher]
- Motaharian E.S., Mahmoodiyeh B., Lorestani S., Sadri M.S., Fard M.M., Fard A.M.M., Amini A., Chem. Rev., 2021, 3:171 [Crossref], [Google Scholar], [Publisher]
- Alimoradzadeh R., Mokhtare M., Agah S., J. Age., 2017, 12:78 [Google Scholar], [Publisher]
- Alimoradzadeh R., Mirmiranpour H., Hashemi P., Pezeshki S., Salehi S.S., Neurology Neurophys., 2019, 10:1 [Google Scholar], [Publisher]
- Abdolrazaghnejad A., Banaie M., Safdari M., J. Emerg. Med., 2018, 2:1 [Google Scholar], [Publisher]
- Akhlaghi N., Payandemehr P., Yaseri M., Akhlaghi AA., Abdolrazaghnejad A., Emerg. Med., 2019, 73:462 [Crossref], [Google Scholar], [Publisher]
- Abdolrazaghnejad A., Banaie M., J. Pharma, 2017, 12:180 [Crossref], [Google Scholar], [Publisher]
- Pakniyat A., Qaribi M., Hezaveh DR., Abdolrazaghnejad A., Journal of Acute Disease, 2018, 7:241 [Crossref], [Google Scholar], [Publisher]
- Rahmati J., Fathi H., Sultanova N., Davudov M.M., Danesh HA., J. Otorhinolaryngol. Head Neck. Surg., 2020, 9:86 [Crossref], [Google Scholar], [Publisher]
- Rakei S., Rad H.I., Arbabisarjou A., Danesh H.A., Drug Invent. Today, 2019, 11:3123 [Google Scholar], [Publisher]
- Rakei S., Rad H.I., Irandegani F., Danesh H.A., Drug Invent. Today, 2019, 12:2809 [Google Scholar], [Publisher]
- Danesh H.A., Focus Med. Sci.J., 2018, 4 [Google Scholar], [Publisher]
- Danesh H.A., Saboury M., Sabzi A., Saboury M., Jafary M., Saboury S., J. Islam. Repub. Iran, 2015, 29:172 [Crossref], [Google Scholar], [Publisher]
- Hashemi S.M., Hashemi M., Bahari G., Khaledi A., Danesh H., Allahyari A., Asian Pac. J. Cancer Prev., 2020, 21:2479 [Crossref], [Google Scholar], [Publisher]
- Abdolrazaghnejad A., Banaie M., Safdari M., J. Emerg. Med., 2018, 2:1 [Google Scholar], [Publisher]
- Akhlaghi N., Payandemehr P., Yaseri M., Akhlaghi AA., Abdolrazaghnejad A., Emerg. Medicine, 2019, 73:462 [Crossref], [Google Scholar], [Publisher]
- Abdolrazaghnejad A., Banaie M., J. Pharma, 2017, 12:180 [Crossref], [Google Scholar], [Publisher]
- Pakniyat A., Qaribi M., Hezaveh DR., Abdolrazaghnejad A., Acute Dis., 2018, 7:241 [Crossref], [Google Scholar], [Publisher]
- Mehr S.S., Ramezani A., Kashi M.A., Krimpalis S., Mater. Sci., 2018, 53:14629 [Crossref], [Google Scholar], [Publisher]
- Mehr S.S., Ramezani A., Kashi M.A., Mater. Sci. Mater. Electron., 2018, 29:18771 [Crossref], [Google Scholar], [Publisher]
- Nejad N.H., Saboute M., Hosseini R., Tahoori M., Otukesh H., Compr. Pediatr., 2019, 10:e74359 [Crossref], [Google Scholar], [Publisher]
- Hoseiny-Nejad , Cheraghi T., Nikpour S., Sheikhvatan M., Iran. J. Pediatr., 2018, 28:e63588 [Crossref], [Google Scholar], [Publisher]
- Saboute , Mazouri A., Khalesi N., Hoseiny Nejad N., Razaghian A., Iran. J. Neonatol., 2017, 8:83 [Crossref], [Google Scholar], [Publisher]
- Hoseiny Nejad N., Sadat Sharif A., Otukesh H., Hekmat S., Sakhaei M., Nephrol., 2021, 36:1[Crossref], [Google Scholar], [Publisher]
- Bahoush G., Zarei E., Open Maced. J. Med. Sci., 2020, 8: 233 [Crossref], [Google Scholar], [Publisher]
- Bahoush G., Pahlavani R., Salarinejad S., Zarei E., Case Rep., 2021, 16: 166 [Crossref], [Google Scholar], [Publisher]
- Samimi A., Samimi M., Eng. Ind. Res. 2021, 2:1 [Crossref], [Google Scholar], [Publisher]
- Bidari A., Hassanzadeh M., Naderkhani M., Mesgarha M.G., Mohammad A.P., Azadeh A., Hossein H., Zarei E., Khodadost M., J. Islam Repub. Iran, 2021, 35:1 [Crossref], [Google Scholar], [Publisher]


